In this month’s Journal Club, we explored the impact of post-intubation hypotension for critically ill trauma patients with severe traumatic brain injury (TBI) in the prehospital setting.
Background and Study Objectives
Trauma patients present with a variety of complexities where, notably, those with severe TBI have been demonstrated to have a decreased survival rate. There exist multiple secondary insults that can impact clinical outcome in those with severe TBI including hypoxia and hypotension. The concept of “permissive hypotension” in the trauma setting is well studied although careful consideration is given to patients with cranial and spinal injuries. These patients can present altered with an inability to maintain airway due to decreased GCS often resulting in intubation. The post-intubation period alone can result in hypotension as a complication from physiologic parameters which leads to careful thought to determine safety of intubation particularly in patients with TBI. The objective of this study is to determine whether hypotension during the post-intubation period in patients with severe traumatic brain injury (TBI) is associated with decreased survival in the prehospital setting.
Methods
- Design: Observational cohort study, single center
- Setting: Cambridge, UK, trauma center with 3 HEMS transport systems
- Study period: January 1st, 2015 – December 31st, 2022
Research Question:
- Population: Critically ill trauma patients (Age 16 years and older) with severe TBI (AIS >3)
- Exposure: Postintubation hypotension (SBP < 90 mmHg within 10 min of intubation)
- Outcomes:
- Primary: 30 day mortality in all trauma patients with severe TBI
- Secondary: 30 day mortality in patients with isolated severe TBI
Key Results
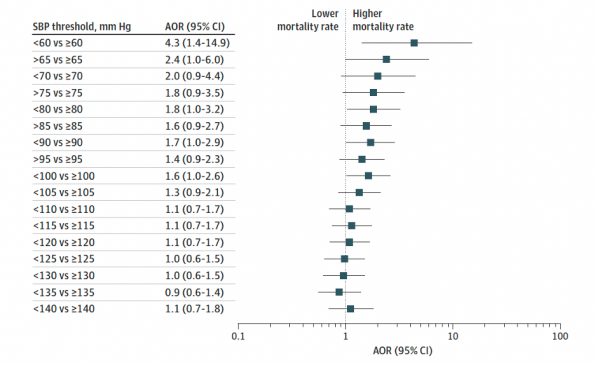
Overall, 555 patients were included in the study where 106 (19.1%) had an incidence of post-intubation hypotension within 10 minutes of establishing an airway. The 30-day mortality rate was 43.3% in the hypotension group and 27.4% in the normotensive group. Further sub-analysis demonstrated an association of increased mortality with hypotension below a systolic blood pressure of 100 (Figure 1). In patients with isolated severe TBI, the adjusted odds ratio of mortality was higher in the hypotensive group compared to patients who were normotensive (AOR, 13.55, 95% CT, 3.65-61.66; p<0.001). For isolated severe TBI, a head AIS score of 5 and associated hypotension had a mortality rate of 94% compared to those with a similar index of injury and were normotensive (37%).
Figure 1 – Adjusted Odds Ratios (AORs) of Death for the Lowest Postintubation Systolic Blood Pressure (SBP) in Patients with Polytrauma and Severe Traumatic Brain Injury.
Strengths
The strength of this study evolves around the real-world prehospital medicine analysis in addition to inclusion of patient centered outcomes (30-day mortality). Multiple layers of sub-analysis were performed to mitigate confounding factors in this complex environment.
Limitations
The biggest limitation of this study is the overall study design whereby an observational cohort does not have the ability to mitigate for all confounding factors. In other words, trauma patients are critically ill and may develop subsequent hypotension from hemorrhagic shock rather than intubation-related causes. Furthermore, this study may not be generalizable to our current system whereby the individuals who participate in patient care within the UK includes both physicians and paramedics. This would lead to a more limited scope of practice within the Canadian EMS system in terms of interventions.
Conclusion
This study emphasizes the importance of preventing post-intubation hypotension in the prehospital setting and suggests a need for updating local protocols to include measures to prevent this occurrence. For example, a target blood pressure prior to orotracheal intubation or inclusion of isolated severe TBI as a contraindication to intubation in the context of hypotension. Ultimately, airway management in the prehospital setting must prioritize hemodynamic stability through the use of limited fluids, pressors and even delayed intubation as suggested mechanisms. Vasopressor support or whole blood may represent a future directive to mitigate occurrence of prehospital hypotension which may result in improved 30-day mortality.

