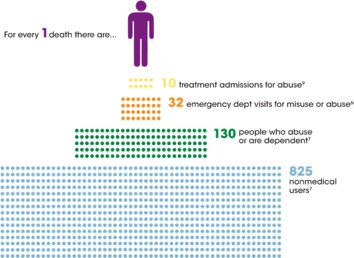
There has been increased publicity and recognition of the hazards associated with opiate use and addiction in recent years, and despite this enhanced recognition, complications from opiate use are continuing to rise. This summary will highlight the opioid epidemic and the scope of this problem in Canada. As Emergency physicians we prescribe opioids to our patients on a regular basis and we commonly deal with patients who are dependent on these medications.
Opioid Epidemic in North America
- Fentanyl has become the leading cause of opioid deaths in Ontario for the first time since Canada’s prescription painkiller crisis begin more than an decade ago.
- From 2005-2011 there was a 250% increase in the number of ER visits in Ontario related to narcotics (including withdrawal, overdose, intoxication, psychosis, harmful use and other related diagnoses).
- Data from the Office of the Chief Coroner shows that opioid-related deaths in Ontario increased dramatically from 2004-2011.
- In particular, deaths related to oxycodone increased from less than 60 in 2004, to 160 in 2011. Deaths related to fentanyl also increased substantially over this period.
- The overall rate of opioid-related mortality increased by 242% between 1991 and 2010.
- There is mounting evidence that physicians certainly over-prescribe narcotics to patients abusing, or whom are likely to abuse these medications, contributing to the associated morbidity and mortality attributed to these drugs.
- This may be an instinctive reaction to the perception that physicians tend to under-treat pain in patients. However, a more appropriate suggestion is that physicians are under-treating pain in patients who require analgesia, and are over-utilizing narcotics in those that do not require it.
- Perhaps the most important step to begin to ameliorate the opioid epidemic is physician recognition, and appropriate prescribing practices.
Safe prescribing in the ED
Centers for DiseaseControl and Prevention (CDC) has partnered with several different groups including (but not limited to) the National Institute on Drug Abuse (NIDA), the Substance Abuse and Mental Health Services Administration (SAMHSA) and the Office of the National Coordinator for Health Information Technology (ONC) to review existing opioid prescribing guidelines and identify common elements associated with safe prescribing practices:
- Conduct a thorough history and physical exam
- Conduct urine drug test, when appropriate
- Consider all treatment options
- Always weight benefits and risks of opioid therapy
- Use opioids when alternative treatments are ineffective
When starting patients on opioids:
- Start them at the lowest effective dose
- Implement pain treatment agreements
- Monitoring pain and treatment progress with documentation: using greater vigilance at higher doses
- Use safe and effective methods for discontinuing opioids
There are 5 commonly used tools for evaluating potential opioid misuse:
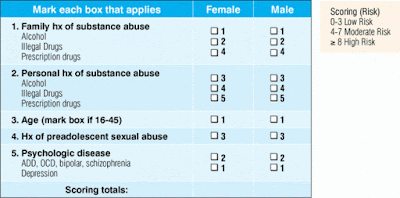 |
| Source: http://www.practicalpainmanagement.com/ |
Medical-Legal issues with opioid prescribing and administration
- Narcotics have an high associated medical-legal risk, and account for 35% of CMPA cases involving medication issues.
- The majority of College complaints allege deficient assessments prior to prescribing, and failure to address risk factors for addiction.
- Over 95% of College complaints involving opioids have unfavourable outcomes for physicians, resulting in verbal or written cautions, or disciplinary action with required remediation or loss of ability to prescribe narcotics.
- All the unfavourable outcomes were for MDs who did prescribe when there were clear red flags for potential abuse.
- All of the Colleges, including the CPSO, refer to the McMaster guidelines for use of opioids for chronic non-malignant pain.
- The CPSO requires Emergency Physicians to include a score for risk of addiction, for example the Opioid Risk Tool (ORT).
Suspicions for opioid dependence
- Enquire with your patient if they have received narcotics in the last 30 days.
- Note that: it is a federal offence not to disclose this information.
- If a patient alleges that their prescription or medications were stolen, ask for a police report prior to prescribing again.
- Obtain any potential collateral information from pharmacy, family physicians or old records.
- Document your assessment and plan clearly (especially when the patient contradicts your findings).
- Quote the CPSO guidelines/McMaster guidelines to patients:
- Because they are on long term narcotics, they need to have one prescriber, have random drug screens, and be on a narcotic contract – which can be terminated by their primary provider if they have received narcotics from another prescriber.
- When prescribing opioids, only give a short supply (for 3-5 days).
- Warn the patient that this is an one-time only event, and that you will be communicating with their primary prescriber (and ensure that you do!).
- Document this conversation, and the expectations for future ER visits.
References