In the first part of this series, we looked at the basics of Extra Corporeal Membrane Oxygenation (ECMO) and its primary indications. In this section, we will discuss the factors that are needed to implement an ED ECMO program and what happens when a code ECPR is called at St. Paul’s hospital in Vancouver, which is currently the only ED ECMO center in Canada.
Expert Opinion:There are many necessary components to a successful ED ECMO program. There needs to be a very well-developed pre-hospital system with strict inclusion and exclusion criteria that paramedics can apply. There also needs to be a number of staff who able to provide ECMO. ECMO provides also need proficiency and expertise. – Dr. Brian Grunau, MD MHSc (Emergency Medicine, St. Paul’s Hospital, University of British Columbia)
Development of a Pre-Hospital System
-
- The design of this system depends on what prehospital system we currently have in place
- Most high performing systems, such as our system in Ottawa use a stay and play paradigm vs a scoop and run paradigm
- If we want to add on ECPR into our system, we need to implement a scoop and run strategy
- This then necessitates the development of protocols that outline strict inclusion and exclusion crieria
- We then need to train paramedics to identify cases that meet inclusion for ECPR so that we are not altering care for patients who are not going to get treatment with ECPR
- We then need to implement strategies for rapid transport of these patients
- We know in literature that scoop and run paradigms have poorer resuscitation quality, poorer CPR fundamentals which then lends to poorer overall outcomes. So we need to ensure good cardiac resuscitation with a focus on fundamentals during extrication and transport
- Role fo simulations
What happens when a “Code ECPR” is called at St. Paul’s Hospital?
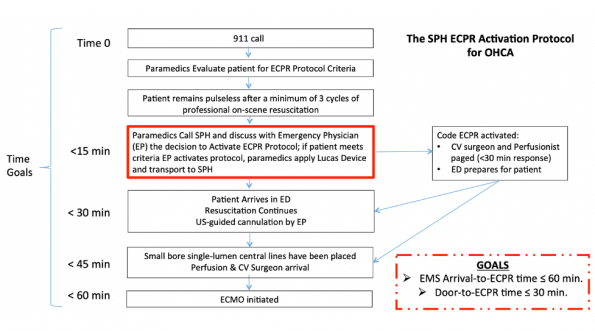
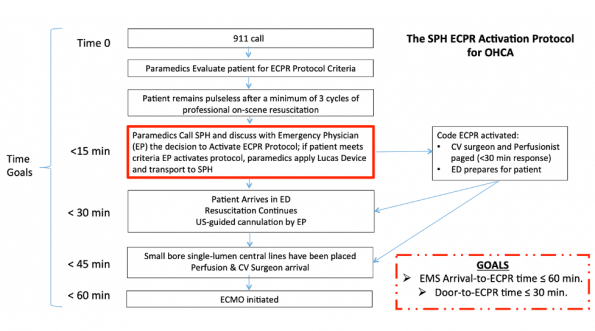
Above is a timeline of the events that occur when a 911 call is received to ECMO initiation at St. Paul’s Hospital in Vancouver. There are two overall time goals:
-
- 911 call to ECPR time of 60 minutes;
- Door to ECPR time of 30 minutes.
Time 0 here is when the 911 call comes in as it provides the best estimate of the time of cardiac arrest. Paramedics will then see if the patient meets specific inclusion criteria (shown below), while continuing on scene resuscitation.

If paramedics deem that the patient meets inclusion criteria, they then call into St. Paul’s to discuss the case with the Emergency Physician (EP).
If the EP is in agreement that the patient meets criteria for ECPR, a code ECPR is called:
-
- This code calls in two teams – a cannulation team and a resuscitation team;
- These two teams work independently of one another;
- The sole purpose of the cannulation team is to gain access and start the ECMO circuit;
- The resuscitation team’s main priority is continuing ACLS care;
- These two teams present to the resuscitation bay and set up prior to the arrival of the patient.

On patient arrival, the patient is then rapidly screened again for additional ECPR inclusion.
-
- While screening is taking place, compressions are continued via the LUCAS device, the cannulation team starts to gain vascular access and the resuscitation team continues typical ACLS level care.
- Once these criteria are confirmed the patient is then set up to the circuit.
Currently, at St. Paul’s hospital, their median 911 to ECMO initiation time is about 60-65 minutes and their door to ECMO initiation time is 18 minutes. These times are not bad but are not comparable to the times shown from the Minnesota group.
Expert Opinion: “In order for an ECPR program to be successful like the Yannopoulous program in Minnesota, the program has to be extremely mature and developed in all realms from prehospital care to ED and Cath lab care to ICU care…Only once these are established and we have our reps in critical care experience can we be proficient at ECPR and navigate issues as they arise…once these fundamental aspects are solid, we may be able to replicate the results from the ARREST trial and that ECPR may be the future of cardiac arrest care…” – Dr. George Mastoras, MD FRCPC (Emergency Medicine, University Health Network, University of Toronto)
Part 4: Future Directions at TOH
This brings us to the last section of this blog post. Here, we are going to take a look at what ED ECMO might look like at TOH.
Expert Opinion: “…[our] ECMO program is still in its infancy and we are far from an ED ECMO program…one of the largest factors is the volume of cardiac arrest patients, which we just don’t have…”– Cari Poulin, RN MN (Nurse Educator at the Civic ED, The Ottawa Hospital)
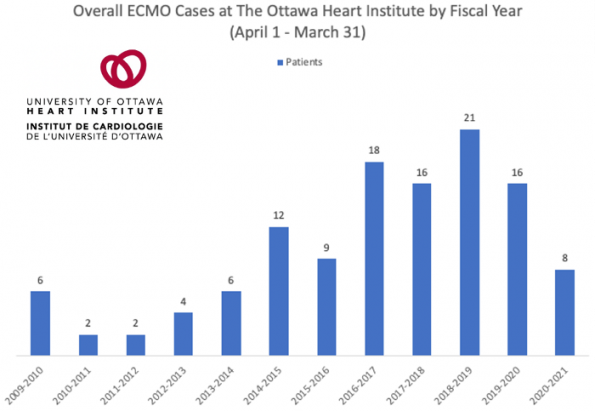
Over the last decade, there has been approximately 114 cases of ECMO. The breakdown of the underlying disease process in these cases is unclear. However, there has been a gradual increase in the number of cases yearly. Even then in Ottawa we currently do not have the ECMO volume compared to other major centers in Canada.
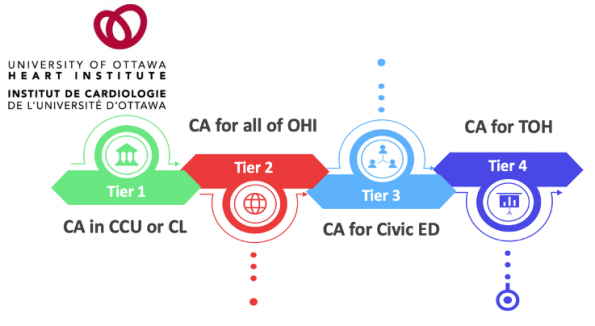
In Ottawa, we are working towards developing this maturity and experience. The Ottawa Heart Institute (OHI) led by Dr. Brock Wilson, currently has a tiered roll out system for ECPR.
-
- Tier 1: Perform ECPR for IHCA that occurs only in the CCU or Cath lab at the OHI.
- Tier 2: Provide ECPR for all IHCA in OHI. This is where we are at now.
- Tier 3: Expand ECPR for cardiac arrests that occur in all of the OHI and in the Civic ED.
- Tier 4: Include ECPR for cardiac arrests to both the civic and general campuses.
Having a roll out like this, will allow us to increase our experience with ECPR, establish expertise and to establish a solid ECPR protocol.
Moreover, there is discussion between a member of the ED Resuscitation Committee about turning the Civic ED into the Cardiac arrest center. Should this occur, we would potentially take all cardiac arrests including those with non-shockable rhythms. To develop this would require a protocol for an EMS bypass to the Civic ED. Once this happens our volumes would increase, and this may give us the necessary exposure we need.
Overall, it will be years until we obtain the necessary volume, exposure, and development of strong prehospital and ECMO protocols for ECPR. We should not expect to see ECPR program landing in an Ontario ED anytime soon.
Expert Opinion: Both Dr. Christian Vaillancourt, an emergency physician and cardiac arrest researcher in Ottawa and Dr. Sheldon Cheskes, believes that it may be higher yield to focus on the fundamentals in improving cardiac arrest survival compared to developing an ED ECMO program. These would include improving rates of bystander CPR, improving rates of bystander AED use, and measuring CPR quality. Both are adamant that all these measures would improve survival far greater than any ECMO program would, assuming it would first be successful. Additionally, the cost of an ECMO program would far exceed community education measures.
Overall Take-Home Messages
-
- ECMO has a role in ARDS in those with refractory hypoxemia and should be considered early on in those patients who are failing conventional management.
- ECMO for COVID-19 is quite limited due to the questionable benefits and inconclusive evidence of ECMO for ARDS in COVID. It should be considered on a case-by-case basis.
- ECMO should be provided for patients with hypothermic cardiac arrest and as EPs on the ground floor, we should initiate our therapies and get early involvement of our colleagues in CSICU and CV surgery.
- ECPR can be considered in OHCA when flow can be initiated within 60 minutes from cardiac arrest.
- For all cases of ECMO, consideration should be placed only for wisely selected patients in a center with an established ECMO program, protocol, experience and expertise
- ED ECMO may be the future of cardiac arrest care, however, we should not expect it in our EDs anytime soon. In the meantime, while we gain critical care experience in ECMO, we should focus on improving fundamentals of cardiac arrest care.
References
- Austin et al., 2020. Outcomes of Extracorporeal Life Support Use in accidental Hypothermia: A Systematic Review. Ann Thoracic Surgery; 110:1926-32
- Barbaro et al., 2020. Extracorporeal membrane oxygenation support in COVID-19: an international cohort study of the extracorporeal life support organization registry. Lancet.
- Bartos et al., 2020. Improve survival with extracorporeal cardiopulmonary resuscitation despite progressive metabolic derangement associated with prolonged resuscitation. Circulation.
- Bougouin et al., 2020. Extra corporeal cardiopulmonary resuscitation in out-of-hospital cardiac arrest: a registry study. European Heart Journal.
- Coombes et al., 2018. Extracorporeal Membrane Oxygenation for Severe Acute Respiratory Distress Syndrome. NEJM
- Coombes et al., 2020. ECMO for Severe ARDS: Systematic Review and Individual Patient Data Meta-analysis. Intensive Care Med.
- Henry., 2020. COVID-10, ECMO, and lymphopenia: a word of caution. Lancet.
- Holmberg et al., 2018. Extracorporeal cardiopulmonary resuscitation for a cardiac arrest: a systematic review. Resuscitation.
- Hsu et al., In press. Extracorporeal cardiopulmonary resuscitation for refractory out-of-hospital cardiac arrest: results of a randomized feasibility trial of expedited out-of-hospital transport. Annals of Emergency Medicine.
- Makdisi and Wang., 2015. Extracorporeal Membrane Oxygenation (ECMO) Review of a Lifesaving Technology. J Thoracic Disl; 7(7):E166-176
- Pasquier et al., 2018. Hypothermia outcome prediction after extra orporeal life-support for hypothermic cardiac arrest patient: The HOPE score. Resuscitation.
- Pasquier et al., 2019. Hypothermia outcome prediction after extracorporeal life-support for hypothermia cardiac arrest patients: An external validation of the HOPE score. Resuscitation.
- Peek et al., 2009. Efficiency and economic assessment of conventional ventilatory support versus extracorporeal membrane oxygenation for severe adult respiratory failure (CESAR): a multicentre randomized controlled trial. Lancet.
- Squires at al., 2016. Contemporary extracorporeal membrane oxygenation therapy in adults: Fundamental principles and systematic review of the evidence. J Thoracic and Cardiovascular Surgery; 152(1):20-31
- Stub et al., 2015. Refractory cardiac arrest treated with mechanical CPR, hypothermia, ECMO and early reperfusion (the CHEER trial). Resuscitation.
- Swol et al., 2018. Extracorporeal Life Support in the Emergency Department: A Narrative Review for the Emergency Physician. Resuscitation
- Yang et al., 2020. Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study. Lancet
- Yannopoulous et al., 2020. Advanced reperfusion strategies for patients with out-of-hospital cardiac arrest and refractory ventricular fibrillation (ARREST): phase 2, single centre, open-label, randomized controlled trial. Lancet.
- World Health Organization (WHO). Interim guidance May 27, 2020. Clinical management of COVID-19.
- Zapol et al., 1979. Extracorporeal Membrane Oxygenation in Severe Acute Respiratory Failure. JAMA