A female in her 70s from a nursing home with a past medical history of dementia, obesity, COPD, and CHF presents to the emergency department with a decreased level of consciousness and shortness of breath. Seven days ago she was assessed in the ER with a diagnosis of aspiration pneumonia and discharged home on Levofloxacin.
Her vitals today are SBP 50/30, P140, R40, T38.4, glucose normal, O2 sat 92% on room air. EMS reports that they were called for respiratory distress with no history of trauma, seizure, allergic ingestion, or vomiting. The history is limited due to the patient’s dementia and decreased level of consciousness. The family notes good quality of life and her documented goals of care include maximal medical therapy without intubation or ICU care.
Her exam shows marked respiratory distress, with poor air entry bilaterally and expiratory wheezes. Cardiac exam is unremarkable, with minimal peripheral edema to the ankles. Abdomen is protuberant, soft, tender only to deep palpation, and not peritonitic.
What are your priorities at this point
At this point, priorities are clearly ABCs. The patient is started on Salbutamol / Atrovent nebulizers, given 2L of fluid, and started on Piperacillin-Tazobactam. She responds to these interventions, becoming more alert and asking for water, with more comfortable breathing and an improvement in her vital signs: BP 105/70, P130, R28, T38.0, O2 sat 97%
A Chest x-ray indicates no significant difference from last week – just evidence of aspiration in the left lower lobe. ECG shows sinus tachycardia, no ischemia. Laboratory investigations are significant for: WBC 42.6, Hgb 111, Lactate of 13.9, VBG showing a pure respiratory acidosis with a pH of 7.03, normal troponin. She is referred to medicine for pneumonia/COPD exacerbation.
What is your Differential Diagnosis?
Given the patient’s past medical problems and current presentation, some things to consider:
- Sepsis
- Hypovolemia
- CHF/Cardiogenic shock: exacerbated by iatrogenic fluids. Cardiomyopathy of sepsis is also a consideration that may be causing a transient worsening of the patients baseline CHF.
- Pneumothorax
- Pulmonary Embolism
Case Progression
A focused POCUS was performed to differentiate these causes and direct further fluid management after 5L of fluid.
The primary concern was that the patient may have been fluid overloaded and the POCUS was performed to evaluate for pulmonary edema. Only one view of each side of the lungs is shown but the other views looked similar.
What is your interpretation?
These images show no evidence of pulmonary edema, pericardial effusion, or pneumothorax. However, while looking at the left lung at the costrophrenic angle, free fluid was incidentally noted around the spleen! Further views of the abdomen were obtained.
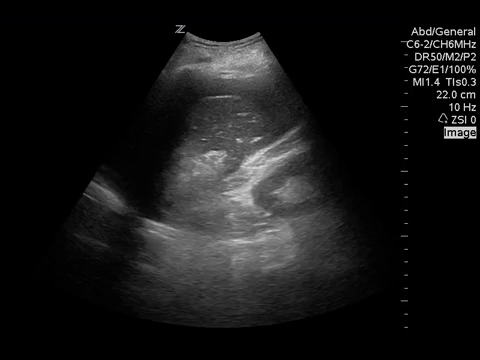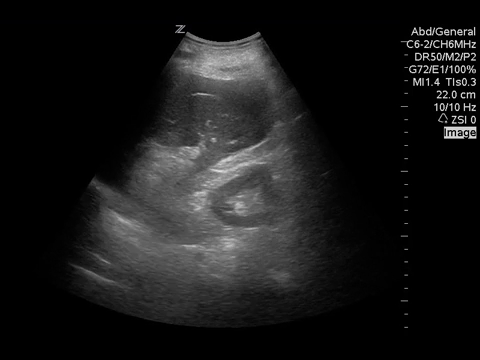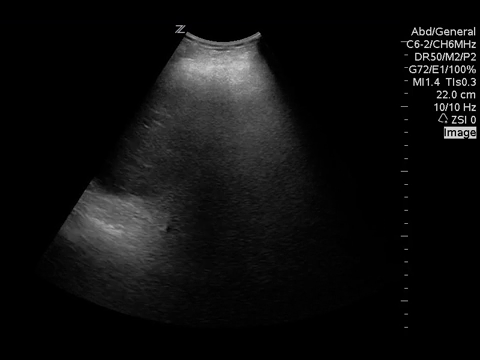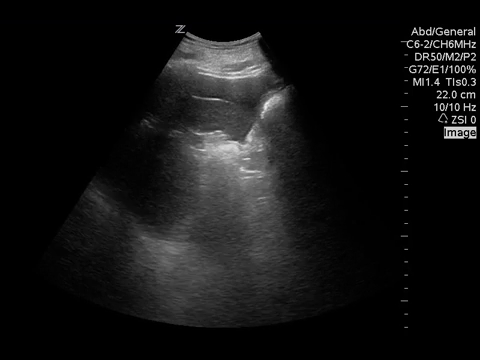
This clip showed a significant amount of free fluid around the spleen, prompting the resident to perform the other views of the FAST to look for more free fluid. A scan of the right upper quadrant was performed next.
These abdominal images of a FAST show significant free fluid and a hyperechoic mass between the liver and gallbladder. While there is clearly recognizable free fluid, the cause of the hyperechoic mass is not a typical finding on a point-of-care ultrasound and needs further investigation!
A more focused examination of the gallbladder was performed as well, due the to abnormal hyperechoic mass in the right upper quadrant. What do you see?
There are multiple gallstones present (which appear as shadows) and a markedly thickened gallbladder wall. The hypereichoic mass appears directly beside the gallbladder.
Resuscitation continued until a CT Chest/Abdomen/Pelvis was obtained. The CT scan confirmed there was no acute lung infection. The CT showed evidence of a gallbladder perforation with a 10 cm abscess directly beside the gallbladder and a large amount of hemoperitoneum from active bleeding from the cystic artery.
Discussion
- Even when the diagnosis is suspected, Point of care ultrasound is a highly valuable tool, in this case in particular:
- In the undifferentiated shock patient to help direct further investigations and management
- To help in the consideration of pulmonary edema, and to help guide fluid resuscitation.
- To help guide your differential diagnosis in patient’s whom the history is unavailable and the physical exam is unreliable.
- Important to consider that gallbladder pathology is a commonly missed cause of undifferentiated shock/sepsis.
Expert commentary
(Dr. Brandon Ritcey, FRCPC, Assistant Ultrasound Program Director)
This is an excellent case by one of our junior residents, who had only recently finished his basic ultrasound training at the time and had no formal training in lung ultrasound! I think this really highlights the fact that these skills can be obtained by anyone, no matter what stage of their career.
I think the most important point demonstrated by this case is to consider gallbladder pathology in the case of undifferentiated sepsis when a good history is unavailable. Through reviewing cases as part of our ultrasound quality improvement program, we have come across many cases where cholecystitis or a perforated gallbladder was found incidentally while performing an abdominal ultrasound in elderly patients in undifferentiated shock. Elderly patients have very friable tissue and can have their gallbladder rupture as the first sign of gallbladder disease, and they often have very poorly localized pain. They also often won’t demonstrate peritonitis due to abdominal muscle atrophy, which makes the clinical exam unreliable. This patient was thought to have a respiratory infection, but thanks to the point of care ultrasound and some great thinking by the resident, the proper diagnosis was found.
The images obtained by the resident are very good. The one extra thing I would have liked to see would be a short axis view of the gallbladder. Something I always recommend to POCUS learners, is when you see something unusual that you can’t identify, image it in more than one plane. This gives you the best chance to figure out what the abnormal structure looks like in 3 dimensions, what it’s attached to, and hopefully what it is. In this case, a short axis gallbladder view would have made it easier to see the gallbladder wall thickening, identify if the stones were really in the gallbladder, and give a better sense of the size of the liver abscess.