On a sweltering night in July, I’m called to see a patient with difficulty breathing. I work in Toronto, where past estimates have placed the number of heat-related deaths at about 120 each year. With Canada heating twice as fast as the world average, that number is likely rising. In Montréal, during 2018, 66 people died during a single heatwave. With greater risks on the horizon, innovative thinking and sustainable change can counteract the drivers of climate change and help to build more resilient communities for a healthier future.
Average temperatures all across Canada are expected to rise by several degrees over the next century (you can look up where you live at climatedata.ca). In the middle of winter, that can be hard to imagine. But as our patients know, the effects can be devastating.
The patient in front of me would certainly have agreed. Maureen (not her real name) was critically ill. She was elderly and lived in an apartment without air conditioning. For a few days, she felt her chest getting heavier, until it seemed as if she was drowning. With enough oxygen, medication, and skillful team members, her breathing gradually eased. She was suffering from heat exhaustion and acute coronary syndrome, but thankfully, stabilized.
Maureen’s story is familiar: the heat and smog of summer are linked to higher risks of death from cardiac and respiratory diseases. Particulates contribute to MIs in adults and exacerbate asthma in children. People affected by wildfires know this from first-hand experience.
The story above was adapted from a newspaper article I wrote for a public audience, so I’ll save you the simplified physiology. You can read a tidy clinical review of heatstroke in NEJM instead. As we know, if your patient’s cooling mechanisms become overwhelmed, they’re on their way to multi-organ dysfunction and failure. There’s more to the clinical picture than that, though.
Older and lower-income adults, like Maureen, are at a disadvantage. They’re often taking medications, or have chronic illnesses that lower their ability to sweat, sustain circulation, stay hydrated, or even physically leave stuffy apartments. Social isolation makes it harder to call for help. Maureen wanted to see her family doctor, but getting there with her walker, by herself, had proved to be an insurmountable challenge.
Even if we’re in different circumstances, we can learn from her story. How hot we feel depends not just on temperature, but on many factors, including airflow, humidity, contact surfaces, and clothing. A lot of the technology around us, even the “smart” gadgets, seem to ignore these important considerations. To cool down more efficiently, we can use fans, cover windows in the daytime, and stay hydrated. If you have AC, dressing for the weather can still improve comfort, save on energy bills, and give others a break from overly chilled spaces. Reducing reliance on AC also avoids blowing hot air outdoors, burdening the electrical grid during peak hours, and contributing to climate change. We want to keep enjoying our summers and prevent them from being intolerable and dangerous for our kids.
That brings me to the key point of this post: climate change and its health effects are not fundamentally tech problems with easy solutions. Instead, this complex puzzle asks us to think about relationships between ourselves, our patients, our health system, our society, and our world, to find innovations for truly sustainable change.
Many of these novel interventions already exist: they are social or behavioural innovations, rather than technological. They answer questions like: how could we have prevented Maureen’s condition? Maureen was not born inherently “vulnerable” to climate change; systemic factors along the way have contributed to her greater risk, as they do for many of us reading this as well.
To explore this, I’d like to present a sample spectrum of transformative actions for sustainable change. Why a spectrum? Because, as Canadian climate scientist Dr. Katherine Hayhoe has said, in tackling the complex issue of climate change, what we need is not a “silver bullet”, but “silver buckshot”. Not a magical cure, but many collective efforts that together build a durable shift.
Sustainable change
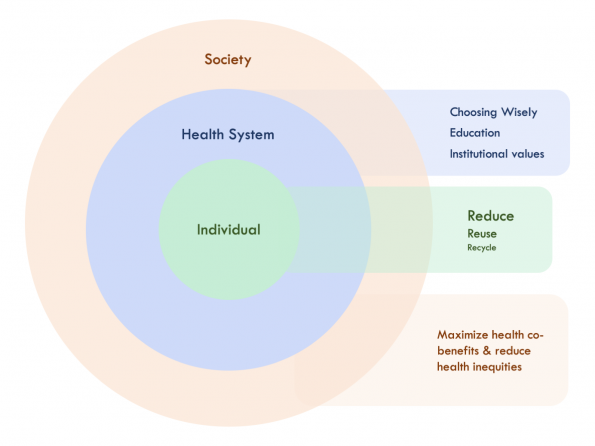
Individual
- Measure your footprint using this Canadian tool to find out where you can make the biggest impact. For most of us, this presents opportunities to improve our travel, diet, and energy use at home.
- If you’re trying to make a personal change (we all know it’s hard), take a listen to this podcast on how to build better habits.
Healthcare System
- Choosing Wisely, because unnecessary tests and treatment = unnecessary CO2.
- Education, because climate change will become an emergency. Some great tools can be found at cape.ca for patients and health professionals (English, Français).
- Institutional values should align with our overarching goals of addressing societal needs and improving health. That’s as true for your hospital as it is for your health ministry. Ask your health system leaders about what they’re doing to mitigate and adapt to climate change. Don’t have an answer? Send them to CCGHC, SSE, or Greening Healthcare for resources.
- If institutional values are aligned (great!), how will their strategies benefit communities and disadvantaged groups? Many approaches to helping patients adapt to climate change lie upstream of the ED: as providers on the front line, we can make the crucial links to resources for addressing the causes of vulnerability. Innovative approaches can be simple. For Maureen, the straightforward act of connecting her with a social worker or housing support services can have a major impact on her future health.
Society
- The health sector has a responsibility to act and many opportunities to do it. Here are the latest Lancet Countdown recommendations for what we can do in Canada (Français, English, All). As trusted voices, we can have a positive influence on public understanding of the problem and motivate policy-makers to act.
- Most importantly, the structural factors that contributed to Maureen’s “vulnerability” are some of the same ones that are fueling climate change. That’s a lot to cover in one blog post, so I’m going to let economist Kate Raworth tell you about it in her TED Talk.
Finally, don’t forget to check out all the inspiring work done by other authors and their ideas for personal, health care, and systemic change in this series.
With so much opportunity, this is no time to be discouraged. We can achieve a great deal as individuals but will accomplish even more by amplifying our efforts along with our friends, colleagues, and neighbours. One of the simplest things you can do is to tell others why you care and what you’d like to do about it.
As fellow emerg doc, Dr. Renee Salas said, “The ED proudly sits at the hospital front door as the healthcare system safety net”. By taking action on climate change, we can be the leaders on the front line pushing for more sustainable changes and a better Planet.



