In this post, we aim to highlight the perspectives of family, physicians, the emergency department and pre-hospital medicine in regards to organ donation.
Types of Organ Tissue Donation
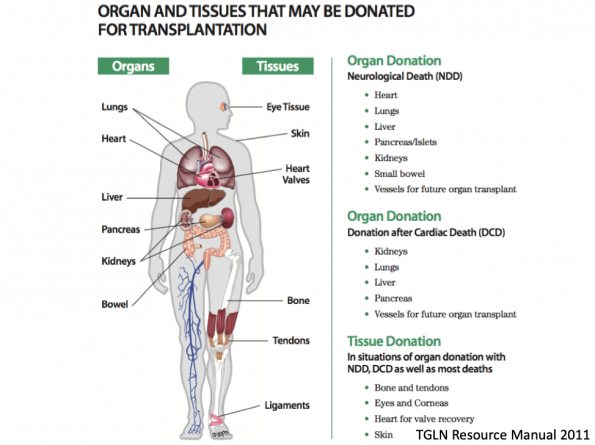
There are 2 main types of deceased organ donation including neurologic determination of death and donation after circulatory determination of death.
Neurologic determination of death includes a very strict set of criteria including physical examination and imaging findings, previously called brain death. Not all non-survivable neurologic injuries are consistent with neurologic determination of death.
Neurological Determination of Death:
- Irreversible loss of capacity for consciousness combined with irreversible loss of all brainstem functions including the ability to breathe
- Non-survivable neurologic injury does NOT necessarily equate to neurologic determination of death
Donation after Circulatory Determination of Death- Modified Maastricht Classification:
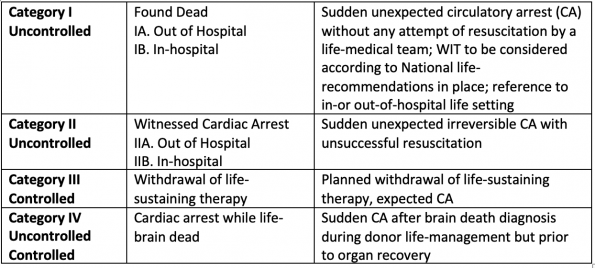
(Modified from table by Thuong et al, 2015)
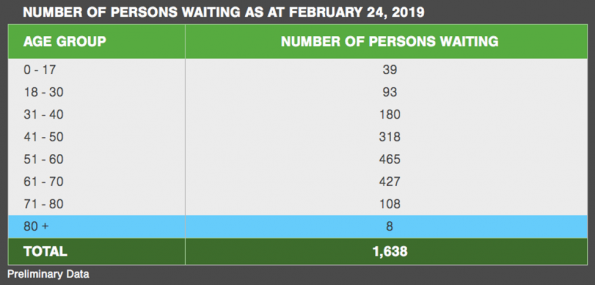
Organ Donor Shortage in Ontario
Click HERE for more statistics on organ donation in Ontario.

Organ Donation Around the World
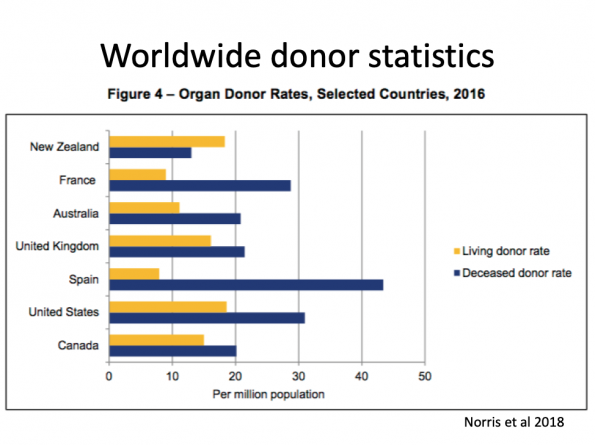
Canada was 19th among 68 countries for deceased organ donation with a rate of 20.1 per million population (Norris et al 2018). The top country was Spain with a rate of 43.4 per million population. There are several possible reasons why this may be.
1) Opt out system
- Shepherd et al (2014) conducted an international comparison of deceased organ donor rates per million population between countries with an opt-in compared to an opt-out system
- Opt-out countries had a 14.24 per million population rate and opt-in countries had a 9.98 per million population rate (p=0.029)
2) Intensive Care to facilitate organ donation
Martinez-Soba et al (2018) did a a retrospective review at 2 Spanish Centers over 4 years where family was approached to discuss organ donation once treatment was deemed futile after brain death.
66% of these interviews occurred in the ED
- 95% of families consented
- 131 patients, 125 consented, 101 developed brain death, 99 actual donors
- ICOD contributed to 33% of donors
- Most significant finding was that in 50% of these patients there had been a decision to not ventilate the patient for therapeutic purposes
Domininguez et al (2017): Retrospective audit of ACCORD-Spain database including 68 hospitals over 6 months.
Family approached to discuss organ donation once treatment futile after brain death
- 257 approached, 174 (68%) consented, 131 developed brain death, 117 donors
- ICOD contributed to 24% of donors
- 30% underwent non-therapeutic intubation and ventilation
A forum was held February 23 to 24, 2015, in British Columbia in conjunction with the Whistler Canadian Critical Care Conference to develop consensus guidelines for donation in Canada and the following guideline was produced:
“Where interventions may potentially cause harm, then risks and benefits and purpose (if strictly for donation) need to be discussed between the MRP, the treating team, and the family.” (Shemie et al, 2017).
3) Uncontrolled donation after circulatory determination of death including (uDCDD) pre-hospital
A study published in 2018 was single center, prospective, observational study of selected patients with in-hospital (IHCA) and out-of- hospital (OHCA) over 2.5 years (Roncon-Albuquerque, 2018). Patients were included if they were 65 year old or younger without significant bleeding or comorbidities with witnessed non-asystolic cardiac arrests. They were triaged to ECPR if they had a reversible cause and high quality CPR lasting < 60 min or they were considered for uncontrolled donation after cardiac death after a ten minute no touch period using normothermic regional perfusion.
- Survival to hospital discharge with full neurological recovery (cerebral performance category 1) occurred in 6/18 (33%) ECPR patients. uDCDD resulted in transplantation of 44 kidneys or roughly 18 per year.
Molina et al (2018) conducted a single‐center observational cohort study that included all patients undergoing kidney transplantation from uncontrolled donation after circulatory determination of death donors over 10 years. All potential kidneys came from patients who had an unexpected out-of-hospital cardiac arrest and who were transferred using ECMO used as a bridge to transplant.
- 237 kidney recipients from uncontrolled cardiac death and 237 kidney recipients using standard criteria
- 10‐year death‐censored graft survival (82.1% vs 80.4%; P = .623)
- Recipient survival (86.2% vs 87.6%; P = .454)
Family and Physician Perspectives
There have been 2 studies looking at family perspective after organ donation.
Kentish-Barnes et al (2019) – France
Qualitative study using interviews with bereaved family members who were approached for organ donation after the death of their relative in 13 ICUs. The interviews took place 11–14 months after the patient’s death and were conducted with 16 relatives of organ donor patients and with eight relatives of non-organ donor patients. The authors found:
- Easier to make decision if loved ones wishes known
- Difficulty understanding brain death diagnosis
- Benefit if donation successful (decreased rates of depression, anxiety, PTSD, and complicated grief)
Knihn et al (2016) – Brazil
Interviews of family members who lost a loved one with severe brain injury that evolved to brain death and had been informed about the possibility of donation but have not authorized it . The interviews occurred at least 6 months after death. 17 families were approached and 15 participated. The authors found:
- Families highlighted the difficult in accepting brain death diagnosis when the heart was still beating
- Recommendation: BEFORE initiation of brain death protocol, team must inform family of process, exams performed, and possible results in clear language.
- Team should inform the family about organ donation only after all members have understood and accepted the death.
Macvean et al (2018) conducted a survey of total of 12 intensivists and three emergency department physicians in Australia were who underwent semi-structured interviews to examine physician attitudes and potential barriers when considering the potential for organ donation. Several common themes emerged:
(1) Related to discussions about organ donation and who is best to carry these out
- Duty of care towards patient
- Involvement of third-party organization such as an organ donation organization important
(2) Determining whether organ donation is part of end-of-life care
- Avoidance of non-therapeutic ventilation
- Some reluctance to follow clinical triggers in the emergency department
Organ Donation in the ED
McCallum et al (2019) conducted a systematic review on organ donation from the Emergency Department. If the 1058 records identified, 25 were included in the systematic review.
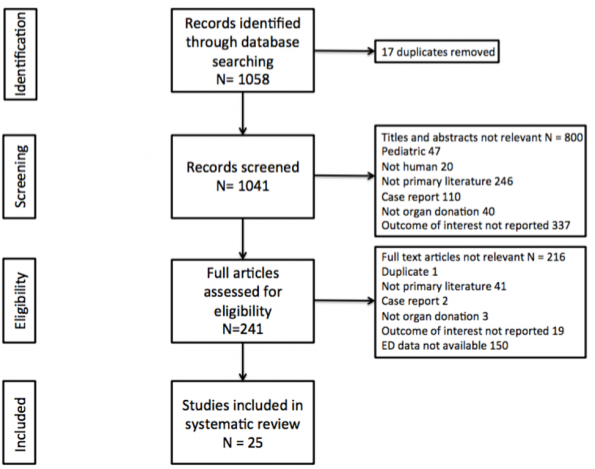
CanadiEM did an infographic on the primary results: https://canadiem.org/emergency-department-organ-donation/
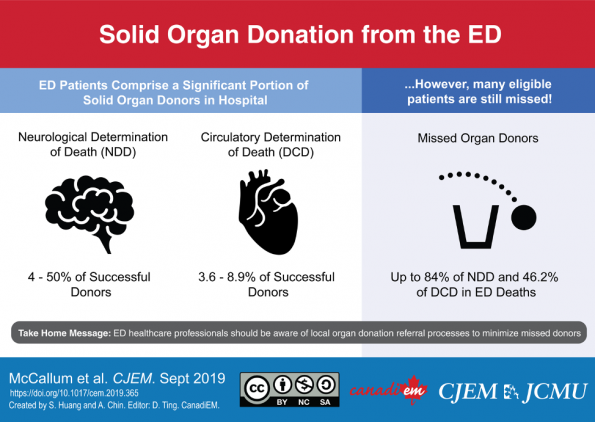
A recent health records and organ donation database review of all patients dying in the Emergency Department at a tertiary academic centre was conducted over a 3-year period (McCallum et al, 2020). 605 people died in the emergency department over the 3-year period. The primary outcome was potential missed solid organ donors. There were ten potential missed solid organ donors. Over the same time period there were 94 successful donors. Therefore, missed potential organ donors in the emergency department could have increased donation by up to 10.6%. All donors were missed due to late referral after withdrawal of life sustaining therapy. Therefore, it is essential that an organ donation organization is contacted prior to withdrawal of life sustaining therapy in the emergency department to ensure potential organ donors are not missed.
Pre-Hospital Perspective
A new pilot project has been developed and implemented over the past couple of years in collaboration between the Ottawa Police Service, Ottawa paramedic service, the Coroners’ Office, and Trillium Gift of Life Network. This pilot has taught 500 police and 500 paramedics about tissue donation and their ability to flag potential tissue donors to the coroner or Trillium Gift of Life Network (Marco Raggi, personal communication, Feb 25, 2019). Stay tuned for results of this initiative!
References:
Dominguez-Gil, B., Coll, E., Elizalde, J., Herrero, J. E., Pont, T., Quindós, B., et al. (2017). Expanding the Donor Pool Through Intensive Care to Facilitate Organ Donation. Transplantation, 101(8), e265–e272. http://doi.org/10.1097/TP.0000000000001701
Gardiner, D. C., Nee, M. S., Wootten, A. E., Andrews, F. J., Bonney, S. C., & Nee, P. A. (2017). Critical care in the Emergency Department: organ donation. Emergency Medicine Journal, 34(4), 256–263. http://doi.org/10.1136/emermed-2016-205941
Huang, Chin, Ting (2019). CanadiEM. Solid organ donation from the emergency department – A systematic review. Available from https://canadiem.org/emergency-department-organ-donation/. Accessed March 7, 2020.
Kentish-Barnes, N., Cohen-Solal, Z., Souppart, V., Cheisson, G., Joseph, L., Martin-Lefèvre, L., et al. (2019). Being Convinced and Taking Responsibility. Critical Care Medicine, 1. http://doi.org/10.1097/CCM.0000000000003616
Knihs, N. D. S., Leitzke, T., Roza, B. D. A., Schirmer, J., & Domingues, T. A. M. (2016). Understanding the experience of family facing hospitalization, brain death, and donation interview. Ciência, Cuidado E Saúde, 14(4), 1520. http://doi.org/10.4025/cienccuidsaude.v14i4.26060
Macvean, E., Yuen, E. Y., Tooley, G., Gardiner, H. M., & Knight, T. (2018). Attitudes of intensive care and emergency physicians in Australia with regard to the organ donation process: A qualitative analysis. Journal of Health Psychology, 1359105318765619. http://doi.org/10.1177/1359105318765619
Martínez-Soba, F., Pérez-Villares, J. M., Martínez-Camarero, L., Lara, R., Monzón, J. L., Fernández-Carmona, A., et al. (2019). Intensive Care to Facilitate Organ Donation. Transplantation, 103(3), 558–564. http://doi.org/10.1097/TP.0000000000002294
McCallum, J., Ellis, B., Dhanani, S., & Stiell, I. G. (2019). Solid organ donation from the emergency department – A systematic review. CJEM : Canadian Journal of Emergency Medical Care = JCMU : Journal Canadien De Soins Medicaux D’urgence, 21(5), 626–637. http://doi.org/10.1017/cem.2019.365
McCallum J, Yip R, Dhanani S, Stiell I. Solid organ donation from the emergency department – missed donor opportunities. CJEM. 2020 Mar 3:1-7. doi: 10.1017/cem.2019.482
Molina, M., Guerrero-Ramos, F., Fernández-Ruiz, M., González, E., Cabrera, J., Morales, E., et al. (2018). Kidney transplant from uncontrolled donation after circulatory death donors maintained by nECMO has long-term outcomes comparable to standard criteria donation after brain death. American Journal of Transplantation, 19(2), 434–447. http://doi.org/10.1161/CIR.0000000000000541
Norris, S. (2018). Organ Donation and Transplantation in Canada, 1–23. Retrieved from http://publications.gc.ca/collections/collection_2018/bdp-lop/bp/YM32-2-2018-13-eng.pdf
Accessed Feb 12, 2019.
Ottawa Police Service (2019). OPS partners with Trillium Gift of Life Network, Ottawa Paramedics, Coroner’s Office to identify potential tissue donors
Available from https://www.ottawapolice.ca/Modules/News/index.aspx?newsId=73601837-1488-4e34-af8b-b391ab9262e4 Accessed Feb 10, 2019.
Roncon-Albuquerque, R., Jr, Gaião, S., Figueiredo, P., Príncipe, N., Basílio, C., Mergulhão, P., et al. (2018). An integrated program of extracorporeal membrane oxygenation (ECMO) assisted cardiopulmonary resuscitation and uncontrolled donation after circulatory determination of death in refractory cardiac arrest. Resuscitation, 133, 88–94. http://doi.org/10.1016/j.resuscitation.2018.10.016
Shemie, S. D., Robertson, A., Beitel, J., Chandler, J., Ferre, E., Evans, J., et al. (2017). End-of-Life Conversations With Families of Potential Donors. Transplantation, 101, S17–S26. http://doi.org/10.1097/TP.0000000000001696
Shepherd, L., O’Carroll, R. E., & Ferguson, E. (2014). An international comparison of deceased and living organ donation/transplant rates in opt-in and opt-out systems: a panel study. BMC Medicine, 12, 131. http://doi.org/10.1186/s12916-014-0131-4
Trillium Gift of Life Network Resoure Manual (2014). Tissue Donation Resource Manual, 2011, 1–62. Available from https://www.giftoflife.on.ca/resources/pdf/Tissue_Donation_Resource_Manual_EN_(final).pdf Accessed Feb 5, 2019.
Trillium Gift of Life Network (2019). https://www.giftoflife.on.ca/en/ Accessed Feb 24, 2019.
Thuong, M., Ruiz, A., Evrard, P., Kuiper, M., Boffa, C., Akhtar, M. Z., et al. (2016). New classification of donation after circulatory death donors definitions and terminology. Transplant International, 29(7), 749–759. http://doi.org/10.1111/j.1600-6143.2009.02739.



