It was during the quiet hours of a night shift that a colleague and I got to talking about the sickle cell patients we see frequently in the Emergency Department. We exchanged stories of the common struggle of getting IV access and how to follow the lead of the patient in what treatments have worked for them in the past. We discussed the immense pain that these patients experience, which at times can be difficult to understand or empathize with, and we were honest with accepting our own bias. The conversation had been inspired by a recent BBC podcast my colleague had listened to featuring Elizabeth Anionwu, a nurse in the UK instrumental in the proper treatment of individuals with sickle cell disease (SSD), helping establish one of the first counselling centres that pioneered the opening of over 30 more centres across the country.
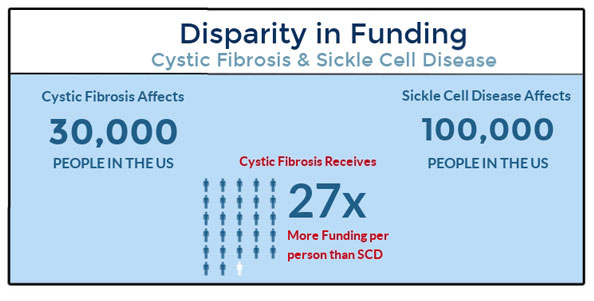
An inherited blood disorder, sickle cell disease is a serious concern of the black community. We often see patients with sickle cell in the ER when they are having a pain crisis. Crises can have unknown triggers but can be caused by dehydration, stress, or even cold temperatures (cue the Canadian polar vortex). These (often) younger patients come to us experiencing pain akin to that of terminal cancer or childbirth but are often stereotyped negatively as “frequent flyers” or drug-seekers. A comparable disease in terms of morbidity and complications is Cystic Fibrosis – which affects 1/3 as many Americans as SSD, but receives 7-11x more funding per patient.
Many hospitals we have protocols that do a good job of taking away much of the potential bias-based barriers to equitably accessing emergency care, but this isn’t the case everywhere and we as individual healthcare providers need to advocate for the use and incorporation of these protocols in an unbiased and timely fashion.
During an interview with the U of T Faculty of Medicine, Dr Isaac Odame reflects:
“One woman with sickle cell disease told us that when she gets intense pain and she needs to go to the emergency room, she puts on makeup. This is so when she appears in the hospital, they will look at her with some respect. Can you imagine you are in pain, and rather than going to seek help, you have to make sure your hair is done and you’re wearing nice clothes?”
Dr Odame has spent much of his career doing research and advocacy work to support sickle cell patients. He was a part of a team that developed a clinical handbook outlining methods in treating these patients that was endorsed by the Ontario Ministry of Health and Long Term Care. Even more locally, we have Dr Ewurabena Simpson, a pediatric hematologist/oncologist at CHEO and investigator at the CHEO Research Institute. Her primary area of interest is in health systems improvement for sickle cell patients and other children or adults experiencing hemoglobinopathies and other chronic hematological conditions and she has been recognized for medical excellence by the Sickle Cell Awareness Group of Ontario.
The work of Anionwu, Odame and Simpson have contributed to making our Emergency Rooms safer places for patients in Sickle Cell crises. It’s important that we each individually take the challenge to pause and reflect as we treat these patients this month and in the months to come and ask ourselves if we are giving them the unbiased care they deserve.
At the end of the articles we’re including a couple reflections from our own staff on what Black History Month has meant to them with the hopes of normalizing a diversity of experiences while encouraging you to reflect honestly and non-judgmentally on your own memories knowing every year is another opportunity to learn and grow a little more.
“As a young black Canadian. I wasn’t taught much about Black History Month (mostly because I grew up in Moose Factory and Nigeria). Fast forward to adulthood I personally feel like BHM is mostly represented by arts (musicians) and sports (basketball). Leaving little room for imagination for young black people.” – Gucci
“I grew up going to predominantly white Catholic schools where there was no focus on Black History Month. Most of what I have learned regarding the history of Black people has come in the last 5 years from the media and from my own research, which I am sure is still not enough.” – Silke


