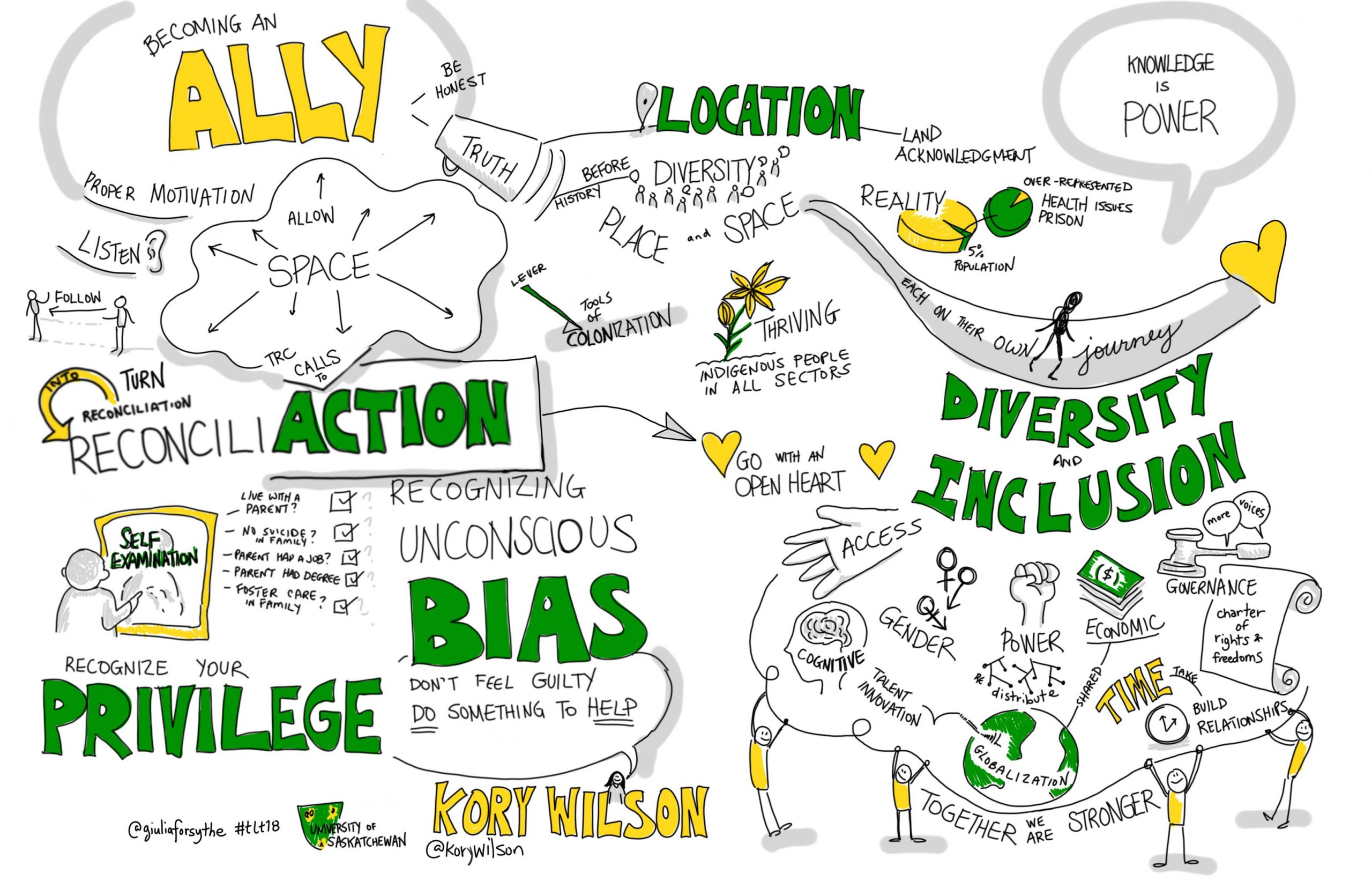
On an individual level, we all have implicit biases. It would be impossible to have a lived experience without having biases. They’re a product of our genetics, environment, opportunities, experiences etc. We develop blindspots that we are often unaware of – and this can have a profound impact on how we perceive the world, treat other people and react to situations around us.
In healthcare – we’re no different. We’d like to think that we see patient’s from a disease perspective only, but this is simply untrue. There is evidence to show that healthcare providers demonstrate the same levels of implicit bias as the general population, and that these biases are very likely to influence the diagnosis and treatment of disease. While we may often be blind to how our biases impact our care – our patients certainly perceive this.
The problem with blindspots is that we’re often not aware of them. It is just like a disease that you’ve never heard of – you can’t diagnose what you don’t know.
We can’t talk about implicit bias ƒezhwithout first acknowledging explicit bias; overt bias/racism. Fortunately, as a society, explicit bias is becoming less prevalent (don’t get me wrong – it is still very much there), and societal tolerance for accepting explicit bias is fading (slowly). Most EDI (equity, diversity and inclusion) work occurs below the surface, however, attempting to address implicit bias – because this is where most the damage is done.
The Sociologic Perspective
It isn’t necessarily our fault, of course. Implicit biases are deeply rooted within our sociologic evolution. We have a tendency towards group formation – spending our early evolutionary phases in close-knit communities, competing with other groups over scarce resources in order to survive. There was safety and assistance by associating with members of your “in group” – collaboration and existence in a mutually beneficial relationship. These groups provided a significant survival advantage, and is one of the reasons our species emerged to become a dominant force on this planet. Systemically, institutions have fostered implicit bias through the same sociologic paradigm.
The thing with our blindspots is that they’re all different, because our life experiences are so vastly unique. So when we talk about inclusion, the perspective is not ‘token recognition’, or that a diverse set of faces is important. It is about the biases and perspectives that person(s) brings. We’re not often cognizant of our blindspots, so it can be hard to act on them, or to advocate for an issue(s) or people(s).
This is why diverse leadership and representation is important. Those various backgrounds are representative of our patient populations, allowing us to have overlapping blindspots so that we can recognize more issues and perspectives that may have been hiding in those blindspots.
I want you to take a moment, and attempt to identify a blindspot that you may have with a simple exercise. On a piece of paper – write down the initials of 6-8 of your ‘inner-circle’; the closest non-family members to you in your life.
Once you’ve done that (click)
Now, I want you to write the following categories across the top:
- Age
- Gender
- Nationality
- Race
- Ethnic Background
- Sexual Orientation
- Disability
- Socioeconomic status
Place a checkmark for each individual that shares a category with you. i.e.: if one person is the same age, place a checkmark. I’ll give you my own example of this exercise:
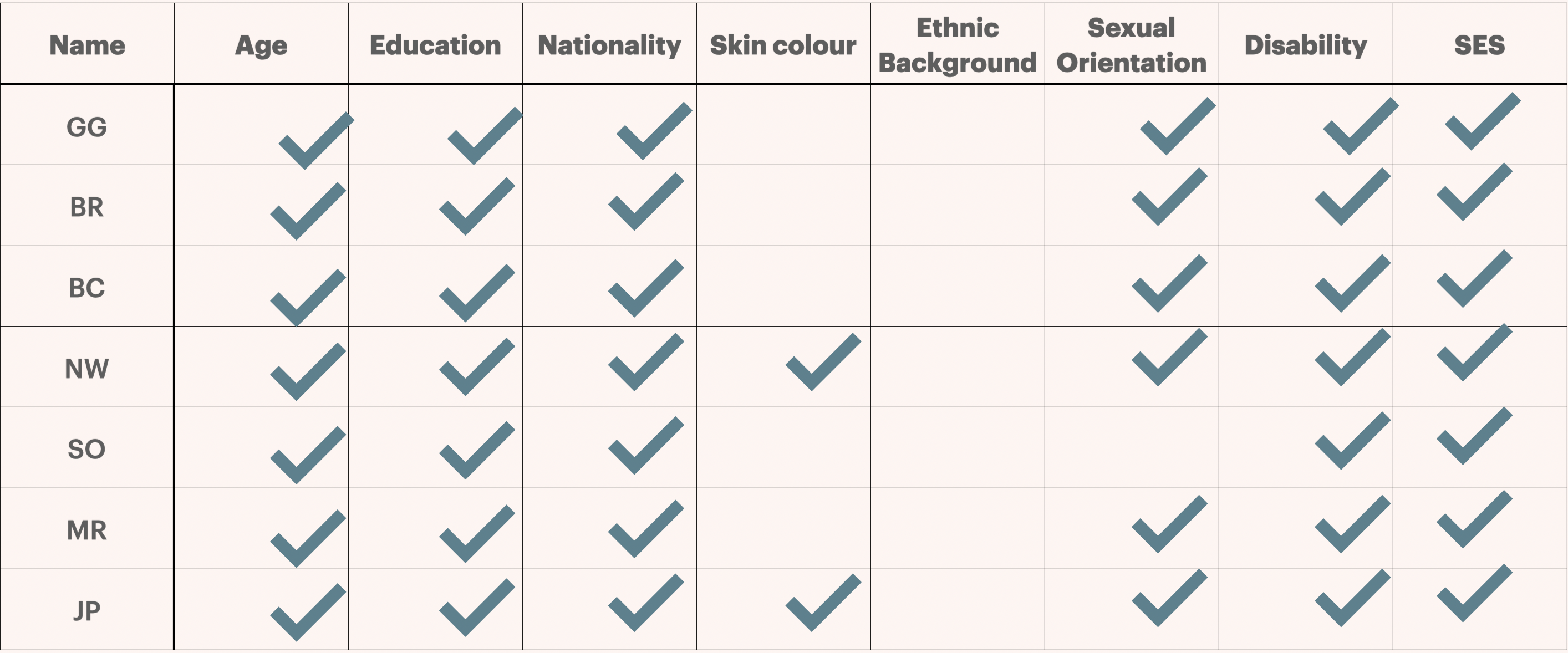
There is certainly a tendency or preference for people to have an in-group bias. Studies demonstrate that people are more likely to engage in cooperation, have positive regard, and be cognizant of one’s emotions with people in the in-group compared to others.
Having an ‘in-group’ doesn’t make you a bad person, it is a natural consequence of existing in a social rubric. However, you can potentially use this as a tool to help identify implicit biases, knowledge gaps, or blindspots. For example – using my own example, I clearly have an in-group that shares significant attributes with myself, entered around people my age, and of similar socioeconomic, educational status and nationality, and I also lack experience with people with disabilities. While this likely exists somewhat subconsciously, because of my experiences and the perspective that I have developed as a result of my ‘in-group’ I likely have biases that exist through a lack of awareness and experience.
Take a second to reflect on your in-group, and attempt to identify if there are any gaps that you may have as a result.
Having implicit bias doesn’t make you a bad healthcare provider or person, but learning to recognize them, and being cognizant of them in your decision making is important.
I’ll give you an example – I am fully aware, that I have bias when it comes to patients with a language barrier. I find it harder to deliver care to these patients, and the frustration of taking a medical history through translation is palpable for me. Being aware of this bias is important, because it allows me to apply a second filter or lens to my decision making at the bedside. I am hyperaware of the fact that I likely order more tests in these patients to compensate for that language barrier, and that I take a little extra time with these patients.
Time for a second reflective exercise – I want you to think for a moment about any implicit biases that you’ve witnessed directly, or any that you have recognized in your self, take a moment to write it down if you find this helpful.
We could probably establish a rather substantial list, but some commonly thought of and recognized examples in healthcare:
- Indigenous patients
- Mental health
- Substance misuse and addictions
- Homeless patients
- Langauge barriers
- Obesity
- Disabilities/perceived higher care needs
- Obesity
- Age
- Sexual identity
- Socioeconomic class
- People of colour
- Chronic pain/chronic pain conditions
- Conflict patients
- Recurrent visits
- Females working in medicine have vastly different experiences than males
- i.e.: mistaken for someone other than the doctor, increased micro aggressions and workplace inequality
- People of colour, minority and marginalized populations also have vastly different healthcare experiences
This is by no means an exhaustive list, but it certainly paints a picture. We all have these biases that we carry, and it influences how we perceive patients – maybe we’re quicker to dismiss because of a cultural expression of pain. Perhaps we’re more attentive to elderly patients, or those with higher health literacy.
We often say that ‘geography is destiny’ when discussing the triaging of patients in the Emergency Department (ED). It is here, that implicit bias can often incur the greatest patient harm. Triage involves significant type I thinking, which can be quick and efficient (important in a busy ED), but is also prone to error and bias. Given a short interaction with a patient, it is very easy for implicit bias (language barrier, perception of pain, etc) to play an influential role in the triage of a patient – and this can lead to significant patient harm.
At the bedside, implicit bias can have a profound impact on our decision making when it comes to testing and diagnosis of disease. There is substantial evidence that demonstrates implicit bias leads to worse care for marginalized populations, i.e.:
- Non-white patients are less likely to be prescribed pain medications (non-opioid and opioid)
- Patients of colour are more likely to be labeled as ‘non-compliant’
- Non-white patients receive fewer cardiovascular interventions and transplants
- Females are less likely to be referred for knee replacement when indicated
- Females are less likely to be diagnosed with COPD
- Elderly patients are less likely to be adequately treated for suicidal ideation
It is no secret that Indigenous patients have experienced explicit and implicit bias through the healthcare system for decades, and that the ramifications of this are still being felt today. The distrust that this has caused them with the healthcare system is a fracture that will be difficult to heal, and requires deliberate and conscious efforts on our part to rectify.
This is a small fraction of the evidence that exists demonstrating bias, but it illustrates a point that has been clear for decades. Implicit bias certainly clouds our judgement, and our ability to provide equitable care.
We have Implicit Biases – now what?
Recognizing that we have implicit biases is important, and attempting to identify where our blindspots are is an important first step in improving the care that we provide our patients. This is obviously quite a hard thing to do – we all want to inherently think that we are good, and that having negative thoughts about certain groups does not fit with the altruistic beliefs of those in healthcare; so it can be hard to address and acknowledge in ourselves that these biases exist.
But they do exist, and having them does not make you a bad healthcare provider or person, identifying these biases is an opportunity to become self-aware and to improve the care that we provide our patients. Learning about ourselves and our patients will help us to provide better individualized care, rather than resorting to stereotypes, or allowing our implicit biases to dictate a patient’s course.
Recognition
When it comes to considering our implicit biases and blindspots – recognition is perhaps the first, and hardest step. The best way to attempt to identify implicit bias in oneself is to listen to your counter-transference, and emotions when it comes to providing care for patients.
If you find yourself getting frustrated or annoying with an interaction, or are deviating from an algorithm or pathway that you tend to have – ask yourself why? Take a moment to process your emotions from an objective ‘birds eye view’.
Listen to patient’s stories, develop rapport, and engage with those outside of your ‘in group’. Take a moment to ask about a marginalized patient’s experience. Engaging patients in their own care has been shown to help physicians identify patients as an individual, rather than being stereotyped.
While the evidence shows that as a species we tend to align ourselves within our ‘in-groups’, sociologic literature also suggests that through exposure, awareness and education that we’re able to expand our in-groups, and develop more empathy towards those in other groups.
Education and Culture Change
If implicit biases are a representation of our blindspots – we need to promote Equity, Diversity and Inclusion groups at a hospital level that help to foster systems of accountability, provide education and knowledge dissemination, and develop helpful policies. These groups should have a systems level approach to their institutions healthcare delivery, to identify gaps and foster positive environmental change to enhance the patient experience. We’re all going to have different gaps in the care that we provide, so this local expertise is critical.
We should improve our patients abilities to communicate with us – through translators, and interpreters that are easy to access and effective. Communication breakdowns are one of the biggest factors involved in a perceived lack of quality care.
We should perceive our patients care and experience through their eyes – to acknowledge their perspectives, and provide more individualized care.
Diverse leadership and representation is important because when we have diverse leadership, we promote an environment beyond a single in-group, and create over-lapping blindspots to provide more representative care to a diverse patient population.