You are working an urgent care shift and you access your ED electronic track-board to pick up the next patient waiting to be seen:
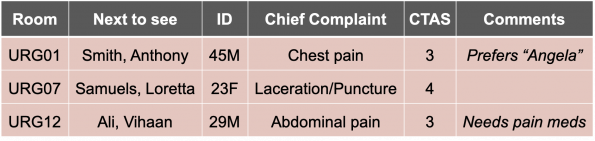
You assign yourself to patient Smith, and notice a helpful comment from your triage nurse stating the patient’s name is Angela. You note the following triage vitals:
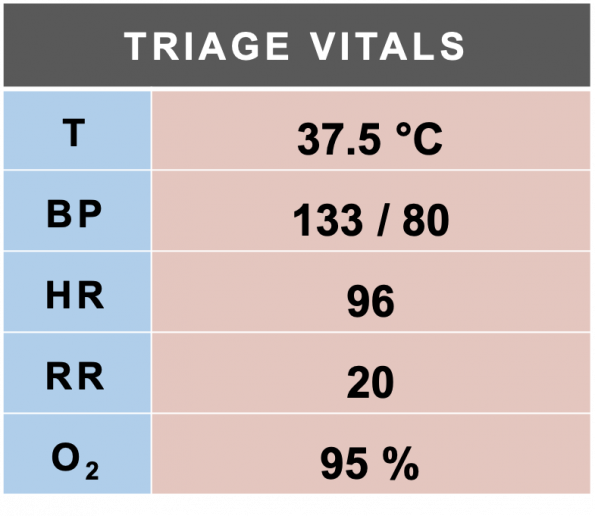
When you meet the patient, you see a middle-aged feminine-presenting patient. You introduce yourself and your pronouns, and learn that your patient’s name is indeed Angela, she uses she/her/hers pronouns, and that she woke up with chest pain this morning.
As you take your history, you run through the HEART score, Wells, and PERC criteria in your head. Angela also has a normal ECG and Troponin, and her HEART score is 1 for her age. She has no unilateral leg swelling/pain/skin changes, hemoptysis, recent trauma or surgery, palpitations, pre-syncope, syncope, and has never had a blood clot before. She does not have any other known medical conditions.
When you ask about hormone use, Angela pauses and appears hesitant. She discloses to you that her sex recorded at birth was male, and she is a transgender (trans) woman. She has been taking two medications as part of her hormone treatment for several years now.
- Cyproterone 25mg P.O. daily
- Estradiol 4mg P.O. daily
Question:
Similar to the use of Hormone Replacement Therapy (HRT) in cisgender (cis) women, does the use of feminizing hormone therapy put trans women at higher risk for venous thromboembolism (VTE)?
Evidence:
Unfortunately, high-quality studies on this topic are lacking. Several reviews have analyzed existing data and have found that the risk of VTE in transfeminine patients taking hormone therapy is comparable to rates of VTE in post-menopausal cis women taking HRT, or in pre-menopausal cis women taking combined oral contraceptives. However, studies had significant heterogeneity in their findings, and results were highly dependent on the formulation of estrogen taken. Oral estrogens are associated with the highest risk:
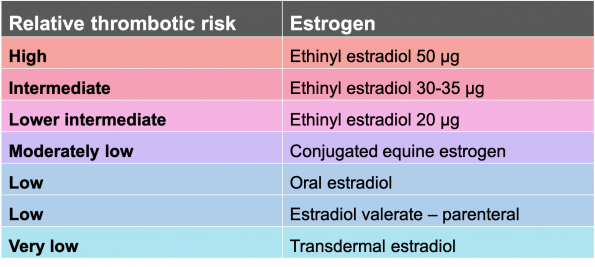
Table 1 | Relative thrombotic risk of estrogenic hormone therapies. Adapted from Connors et al. 2019.
- Oral ethinyl estradiol is the most commonly used form of estrogen in combination oral contraceptives. It confers highest thrombotic risk. It is associated with a 3-fold increase in the risk of VTE and other cardiovascular events. This risk appears to be dose-dependent.
- Oral conjugated equine estrogen is also likely associated with an increased risk of VTE, although perhaps lower risk than ethinyl estradiol.
- Oral estradiol and the injectable estradiol valerate likely confer a reduced risk of VTE compared to ethinyl estradiol and conjugated equine estrogen.
- Transdermal 17-beta-estradiol patch (Estrace) appears to have the lowest risk.
The largest meta-analysis of VTE risk in TGD patients on feminizing hormone therapy included 18 studies and found that overall incidence of VTE was 2-3%, with significant heterogeneity between studies. Prevalence of VTE was increased by age and duration of estrogen therapy.
Some additional considerations:
- For the reasons listed above, ethinyl estradiol and other oral estrogens have become far less prevalent in hormone therapy regimens over the past few years. Nevertheless, there are still patients today who are stable on these treatments.
-
Due to the significant barriers trans people face when accessing care, trans women may have been started on oral estrogens years ago and refill this prescription, without ever having been offered transdermal or other safer estrogen therapies.
-
- Trans people are among some of the most underserved populations in health care, and there are significant barriers to access of timely and safe care. These barriers have been linked with the use of non-prescribed hormones obtained through friends and family, strangers, or the Internet.
- One Ontario study found that up to a quarter of trans patients had ever self-treated with non-prescribed hormones. The emergency clinician should consider the use of non-prescribed hormones when taking a medication history.
- While hormone therapy increases the risk of VTE, absolute risk remains relatively low. Hormone therapy in trans individuals is considered essential, and is associated with lower rates of suicide. For many, the increase in VTE risk is acceptable.
- There are currently no guidelines surrounding withholding hormone therapy in trans individuals diagnosed with a VTE. Withholding estrogen therapy can be very distressing both physically and mentally. Approach this consideration by assessing the risks/benefits of either scenario and discussing these with the patient.
- Hormone therapy with testosterone in patients who were assigned-female at birth (AFAB) does not appear to be associated with an increased risk of VTE.
- Cyproterone – an androgen antagonist – confers a slight increase in risk of VTE, though this is in combination with combined oral contraceptives in cis women. Cyproterone’s contribution to VTE risk in TGD patients has not been studied.
- Spironolactone does not appear to be associated with an increased VTE risk, however, it decreases the efficacy of transdermal estrogen and thus often necessitates the use of oral estrogens.
Case continued:
You opt to order a D-Dimer, which is elevated at 1450 ng/mL. Following a shared-decision making conversation with Angela, you both decide to obtain a CT-PE, which reveals a segmental pulmonary embolism. You start her on anticoagulation and discuss the pros and cons of stopping her hormone therapy with her. Angela is not prepared to stop her medication right now. She feels the adverse effects this will have on her wellbeing and quality of life outweigh the risk of recurrent thrombosis. You agree together that she will continue her hormone therapy in addition to her new anticoagulant until she is able to discuss this further with her thrombosis doctor at follow-up. You also recommend that she discuss transitioning to a transdermal estrogen formulation with her family doctor or endocrinologist. She is discharged with a prescription for Apixaban.
References:
- Asscheman, H. et al. A long-term follow-up study of mortality in transsexuals receiving treatment with cross-sex hormones. European Journal of Endocrinology 164, 635–642 (2011).
- Bourns, A. Guidelines for gender-affirming primary care with trans and non-binary patients. (2021).
- Connors, J. M. & Middeldorp, S. Transgender patients and the role of the coagulation clinician. Journal of Thrombosis and Haemostasis 17, 1790–1797 (2019).
- Getahun, D. et al. Cross-sex Hormones and Acute Cardiovascular Events in Transgender Persons. Ann Intern Med 169, 205–213 (2018).
- Gialeraki, A., Valsami, S., Pittaras, T., Panayiotakopoulos, G. & Politou, M. Oral Contraceptives and HRT Risk of Thrombosis. Clin Appl Thromb Hemost 24, 217–225 (2018).
- Goldstein, Z., Khan, M., Reisman, T. & Safer, J. D. Managing the risk of venous thromboembolism in transgender adults undergoing hormone therapy. J Blood Med 10, 209–216 (2019).
- Khan, J. Venous Thrombotic Risk in Transgender Women Undergoing Estrogen Therapy: A Systematic Review and Metaanalysis. doi:10.1373/clinchem.2018.288316.
- Kotamarti, V. S., Greige, N., Heiman, A. J., Patel, A. & Ricci, J. A. Risk for Venous Thromboembolism in Transgender Patients Undergoing Cross-Sex Hormone Treatment: A Systematic Review. J Sex Med 18, 1280–1291 (2021).
- Meriggiola, M. C. & Gava, G. Endocrine care of transpeople part II. A review of cross-sex hormonal treatments, outcomes and adverse effects in transwomen. Clin. Endocrinol. (Oxf) 83, 607–615 (2015).
- Rotondi, N. K. et al. Nonprescribed hormone use and self-performed surgeries: ‘do-it-yourself’ transitions in transgender communities in Ontario, Canada. Am J Public Health 103, 1830–1836 (2013).
- Safer, J., Klonkle, B. Caring for Transgender Individuals at Risk for Thrombosis. Foundation for Women & Girls with Blood Disorders. Webinar available at: https://www.fwgbd.org/education/archived-webinars/caring-for-transgender-individuals-at-risk-of-thrombosis.
- Seal, L. J. et al. Predictive markers for mammoplasty and a comparison of side effect profiles in transwomen taking various hormonal regimens. J. Clin. Endocrinol. Metab. 97, 4422–4428 (2012).
- Totaro, Maria, et al. Risk of Venous Thromboembolism in Transgender People Undergoing Hormone Feminizing Therapy: A Prevalence Meta-Analysis and Meta-Regression Study. Frontiers in endocrinology, 1471 (2021).
- Winter, S. et al. Transgender people: health at the margins of society. The Lancet 388, 390–400 (2016).
- Turban, J. L., King, D., Kobe, J., Reisner, S. L. & Keuroghlian, A. S. Access to gender-affirming hormones during adolescence and mental health outcomes among transgender adults. PLOS ONE 17, e0261039 (2022).
- Arnold, J. D., Sarkodie, E. P., Coleman, M. E. & Goldstein, D. A. Incidence of Venous Thromboembolism in Transgender Women Receiving Oral Estradiol. J Sex Med 13, 1773–1777 (2016).