Emergency medicine is a fast-paced realm where paramedics and medical professionals must make split-second decisions that often mean the difference between life and death. In this high-stakes environment, understanding and respecting patient preferences while upholding ethical principles are paramount. This article delves into the crucial role of paramedics in ensuring patients’ choices are honoured and explores the ethical considerations surrounding resuscitation decisions. With a focus on verbal DO NOT RESUSCITATE (DNR) orders, we illuminate the importance of patient-centred care, ethical decision-making, and the potential transformation of emergency medical practice.
The Weight of Unspoken Wishes
Imagine a scenario: a serene morning disrupted by an emergency call. Paramedics rush to the scene of a cardiac arrest. The patient’s spouse frantically informs them that the patient had explicitly communicated a desire to forgo resuscitation efforts. This verbal instruction, however, lacks the formality of a documented DNR order. This situation reflects a recurring issue – countless patients have unspoken preferences, yet only a fraction possess the necessary documentation to ensure their wishes are respected.
The Disconnect: Patient Preferences and Documentation
Recent research underscores a disconcerting discrepancy between patient preferences and documented wishes. A study conducted in Southwestern Ontario found that a staggering 86% of emergency department patients who preferred no resuscitation in the event of cardiac arrest were unaware of the existence of the Ministry of Health’s DNR confirmation form (1), and in another study 95% were not in possession of the form (2). This gap between patients’ choices and their knowledge of available documentation raises significant concerns about the extent to which patients’ preferences are being acknowledged (3).
“A staggering 86% of emergency department patients who preferred no resuscitation were unaware of the Ministry of Health DNR confirmation form”
Navigating Ethical Waters
Central to medical practice are ethical principles that guide healthcare professionals in their interactions with patients and their decision-making. The Advanced Life Support Patient Care Standards (ALS-PCS) offer clear directives for consent to treatment, affirming that if a patient is incapable of providing consent, paramedics must honour a prior capable wish regarding the proposed treatment. Within the realm of resuscitation, this implies a duty to respect a patient’s decision to forego resuscitation if it has been expressed (ALS-PCS v5.2, July 10, 2023).
Further bolstering the importance of patient autonomy, the Health Care Consent Act (4) empowers substitute decision-makers, typically family members, to act on behalf of the patient, adhering to their previously expressed wishes. These ethical tenets accentuate the significance of patient-centered care, underlining the responsibility of healthcare providers to honour patients’ autonomy, even during critical moments.
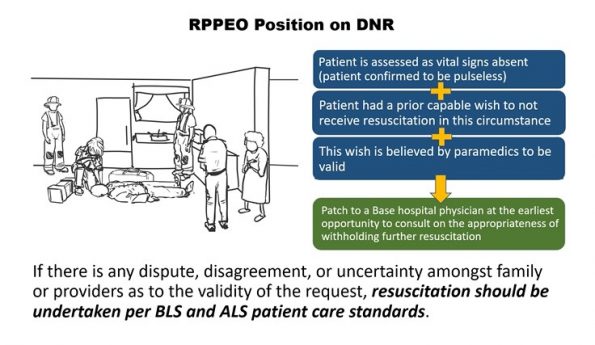
In April this year, RPPEO issued a Medical Advisory indicating the base hospital’s position on the acceptance of verbal and written DNR from substitute decision-makers. With the ethical dilemma of respecting patient wishes while navigating the Standards, RPPEO proposes patching to a Base Hospital Physician to consider withholding resuscitation.
Empowering Paramedics: Bridging the Gap
The RPPEO is taking proactive steps to address this ethical conundrum. Recognizing the complexities faced by paramedics, the RPPEO advocates for the acceptance of all valid expressions of DNR wishes – whether conveyed through a written document or verbal communication from a substitute decision-maker. This approach acknowledges the pivotal role paramedics play in upholding patient preferences and aligns seamlessly with the broader ethical framework of patient autonomy.
Progressive Change in Paramedic Practice
In collaboration with Ontario’s ground ambulance Medical Advisory Committee (MAC), the RPPEO has proposed a crucial amendment to the Basic Life Support Patient Care Standards (BLS-PCS) DNR Standard. This proposed amendment aims to grant paramedics the authority to consider all valid and appropriate expressions of a patient’s wish to withhold resuscitation. While awaiting official endorsement from the Ministry of Health, the RPPEO remains dedicated to refining paramedic practice in scenarios where patients’ preferences for no resuscitation are known.
“RPPEO has proposed a crucial amendment to the Basic Life Support Patient Care Standards … to grant paramedics the authority to consider all valid and appropriate expressions of a patient’s wish to withhold resuscitation”
A Path Forward: Honoring Patient Choices
The RPPEO’s stance on DNR seeks to empower paramedics to align their actions with patients’ desires. According to this approach, if a paramedic encounters a patient with absent vital signs and becomes aware of the patient’s prior expressed wish to avoid resuscitation, a patch to a Base Hospital Physician (BHP) can be initiated for consultation. This consultation safeguards the decision-making process, focusing on upholding ethical and medical standards while respecting the autonomy of patients.
The Crucial Role of Compassion
Paramedics serve as the compassionate faces of the medical field, often being the first responders during critical moments. Your pivotal role demands that you navigate the delicate balance between life-saving interventions and the profound significance of patient preferences. This challenge encapsulates the essence of compassionate healthcare, where the human element is intertwined with medical science.
Conclusion: A Fusion of Ethical Practice and Patient-Centred Care
In the ever-evolving landscape of emergency medicine, the imperative of patient choice and ethical considerations cannot be overstated. The alignment of paramedic practice with patient preferences, particularly in the realm of resuscitation decisions, epitomizes the core principles of medical ethics. As the RPPEO leads the way in embracing patient-centred care, the medical community inches closer to achieving a harmonious equilibrium between life-saving interventions and the respect for patients’ autonomy.
The transformation of emergency medical care into a human-centred practice, where patients’ voices are both heard and honoured, is a testament to the unwavering commitment of paramedics and other medical professionals. Armed with empathy, knowledge, and a deep understanding of ethical principles, these dedicated individuals stand at the forefront of change, working to always put patient preferences at the heart of emergency medical practice.
References
-
- Lipkus, M., Manokara, T., Van Aarsen, K., & Davis, M. (2019). P086: Awareness and barriers to access of a Ministry of Health mandated ‘Do Not Resuscitate’ confirmation form: An interim analysis. Canadian Journal of Emergency Medicine, 21(S1), S94-S95. doi:10.1017/cem.2019.277
- Rose Mengual, Michael Feldman and Gord Jones (2007). Implementation of a novel prehospital advance directive protocol in southeastern Ontario. CJEM, 9(4): 250-9. https:// pubmed.ncbi.nlm.nih.gov/17626689/
- Grudzen CR, Koenig WJ, Hoffman JR, Boscardin WJ, Lorenz KA, Asch SM (2009). Potential impact of a verbal prehospital DNR policy. Prehosp Emerg Care. Apr- Jun;13(2):169-72. doi: 10.1080/10903120802471923. PMID: 19291552
- Health Care Consent Act (1996). S.O. 1996, CHAPTER 2, SCHEDULE A. Retrieved from https://www.ontario.ca/laws/ statute/96h02


