In part one of this two-part series, we took a bite out of Lyme disease and Malaria (see what we did there?). In this part, we’ll be covering African tick-bite fever, African sleeping sickness, Dengue, Chikungunya, and Zika. Fever in the returning traveler is always a challenging presentation, so we hope that this series will serve as a cheat sheet for these more common travel-related diseases that should be on your radar.
As a reminder, Table 1 is your cheat sheet for all diseases talked about in this series:
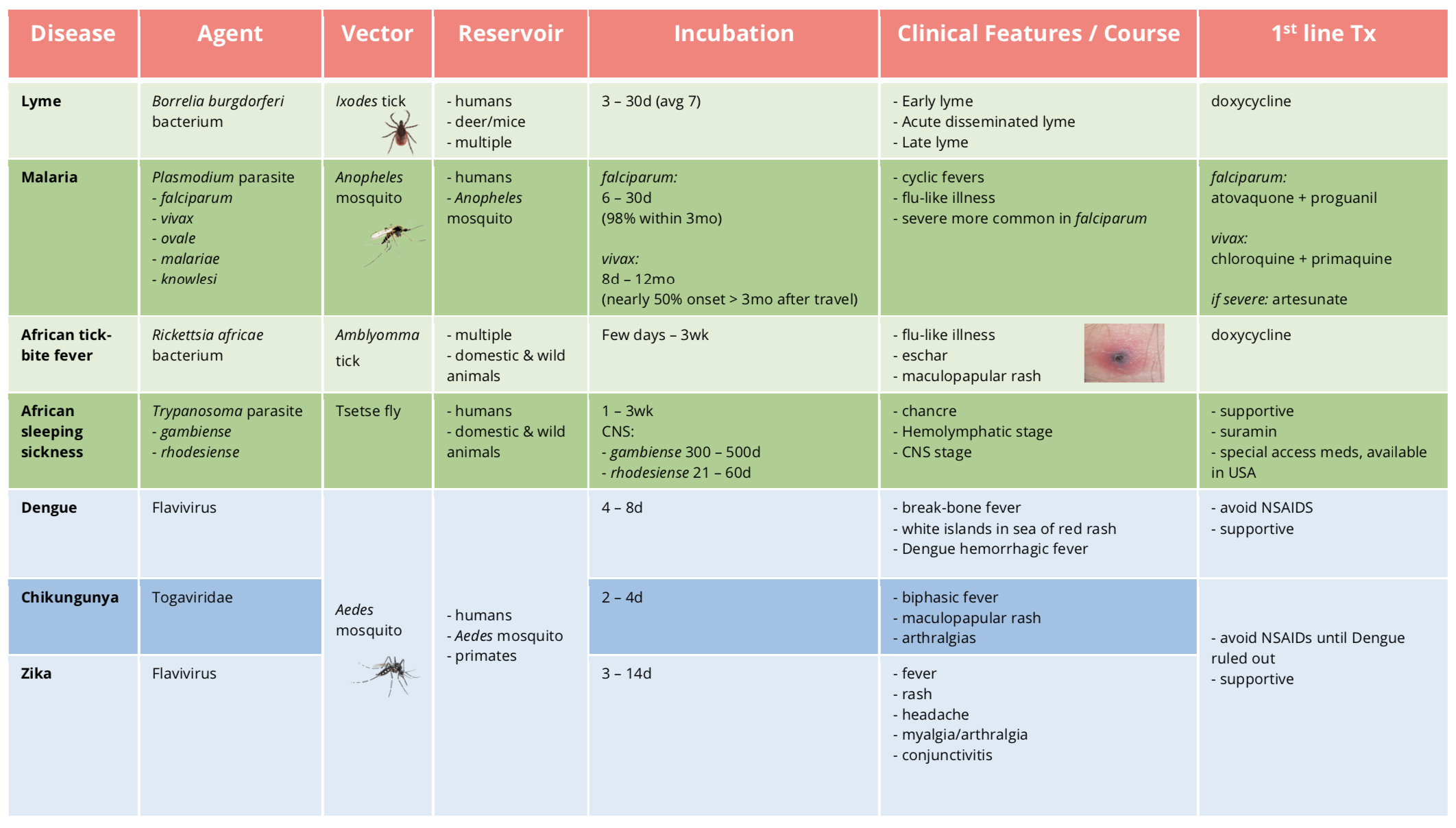
Table 1 | Summary of agent, vector, reservoir, incubation period, common symptoms, and first-line treatment for vector-borne illness causing fever and rash. d: day(s), wk: week(s), mo: month(s).
African tick-bite fever
- Vectors
- Most common: ticks (Amblyomma tick), fish, mites, and fleas
- Agent: bacteria
- 7 antigenic groups of Rickettsia
- Scrub Typhus and Spotted fever
- 18 subtypes of spotted fever
- African tick-bite fever: Rickettsia africae
- Animal reservoirs
- Rodents, deer, dogs, fish, cats, ruminants, wild boar, flying squirrels
- Presentation:
- Flu-like illness
- Rash:
- Eschar
- Maculopapular, vesicular, petechial rash
- Regional lymphadenopathy
- Subacute neuropathy and myocarditis less common
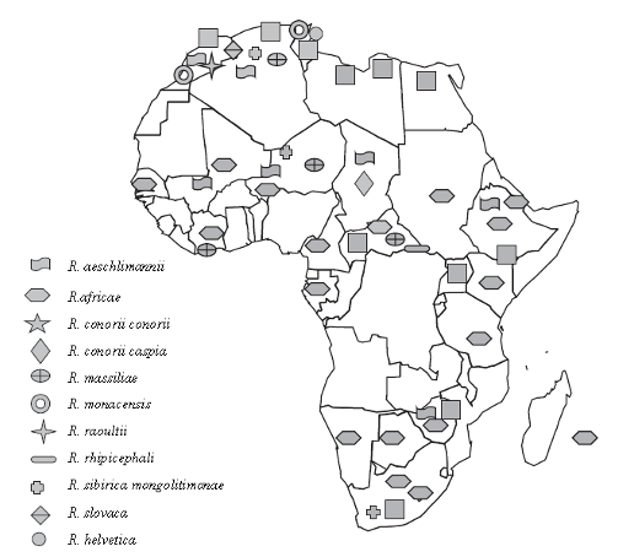
Figure 1 | Distribution of Rickettsial disease in Africa. From Cazorla et al (2008).
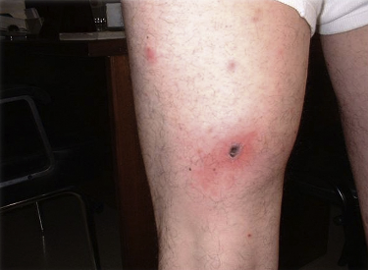
Figure 2 | Example of eschar seen in Rickettsial disease. From Faccini-Martınez et al (2014).
- Diagnosis
- Serologic testing with PCR
- Swab of lesion for PCR analysis
- Treatment
- Doxycycline x 1 week
- Chloramphenicol or azithromycin (children)
African sleeping sickness
- Vector:
- Tsetse fly (Glossina spp.)
- Agent: parasite
- Trypanosoma rhodesiense
- Trypanosoma gambiense
- Transmission
- Bite from Tsetse fly
- Bloodborne and congenital rare
- Reservoir
- domestic wild animals
- Diagnosis
- microscopy
- PCR
- serology
- samples:
- lymph nodes
- CSF for staging
- chancre fluid
- bone marrow
- blood cultures
- Treatment: depends on the region and local availability. For details, click here!
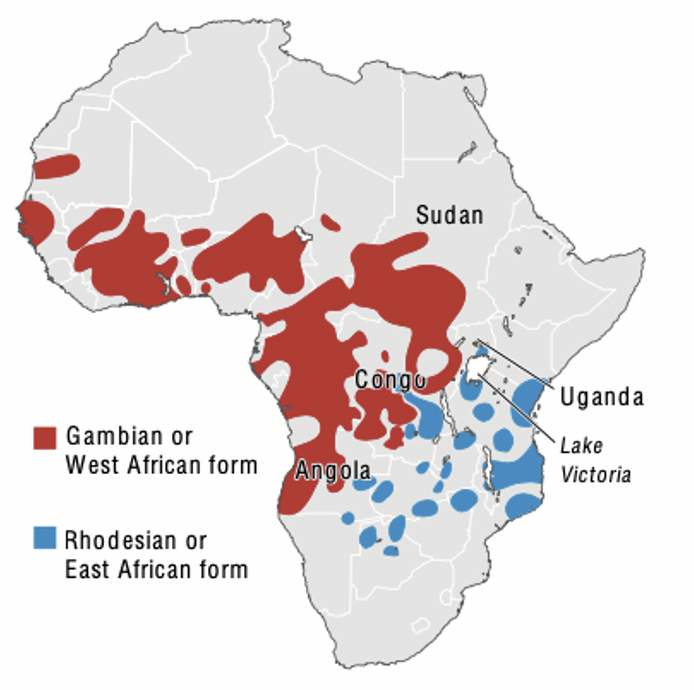
Figure 3 | Distribution of Trypanosoma rhodesiense and gambiense. From Lundkvist et al (2004).

Figure 4 | features of African sleeping sickness.
Dengue
- Vector
- Aedes aegypte
- Aedes albopictus
- Agent
- Flavivirus 1, 2, 3, or 4
- Transmission
- Bite from infected mosquito
- Bloodborne transmission
- Perinatal near birth (likely not congenital)
- Breast milk
- No documented sexual transmissions
- Presentation
- 40 – 80% asymptomatic
- If patients are symptomatic, there are three phrases: Febrile, Critical and Convalescent
- Febrile Presentation:
- ‘Break-bone fever’ (lasts 2-7 days) – severe bony pain, myalgias
- Severe headache with retro-orbital pain
- Severe myalgia & arthralgias
- ‘Island of white’ rash often appears after defervescence (spares palms & soles)
- Critical presentation: Dengue Hemorrhagic Fever
- 4 criteria:
- Increased vascular permeability
- Thrombocytopenia
- Fever lasting 2-7d
- Spontaneous bleeding
- Hepatitis, myocarditis, pancreatitis, encephalitis are possible but unlikely
- Dengue shock syndrome = hypotension, irreversible, shock death
- 5% life-threatening (<0.5% with treatment)
- 4 criteria:
- Convalescent
- Fluid resorption, hemodynamic stability, hematocrit stabilizes
- Rash may desquamate and become pruritic
- Diagnosis
- History: endemic area within 2wks of symptom onset
- Labs: thrombocytopenia, hyponatremia, elevated AST/ALT, normal ESR
- Confirmation
- Early (up to 7d of fever onset): single drum sample RT-PCR or NS1 antigen
- Late (>7d after fever onset): ELISE IgM and IgG
- Can have cross-reactivity with other viruses, including Zika, Chikungunya, West Nile, Yellow Fever, and Japanese Encephalitis.
- Treatment:
- Treatment is almost entirely supportive – AVOID ASA/NSAIDs
- Fever & pain – acetaminophen, sponge baths
- Severe – ICU
- platelets not beneficial
- steroids not beneficial
- Two vaccines are currently in phase 3 clinical trials
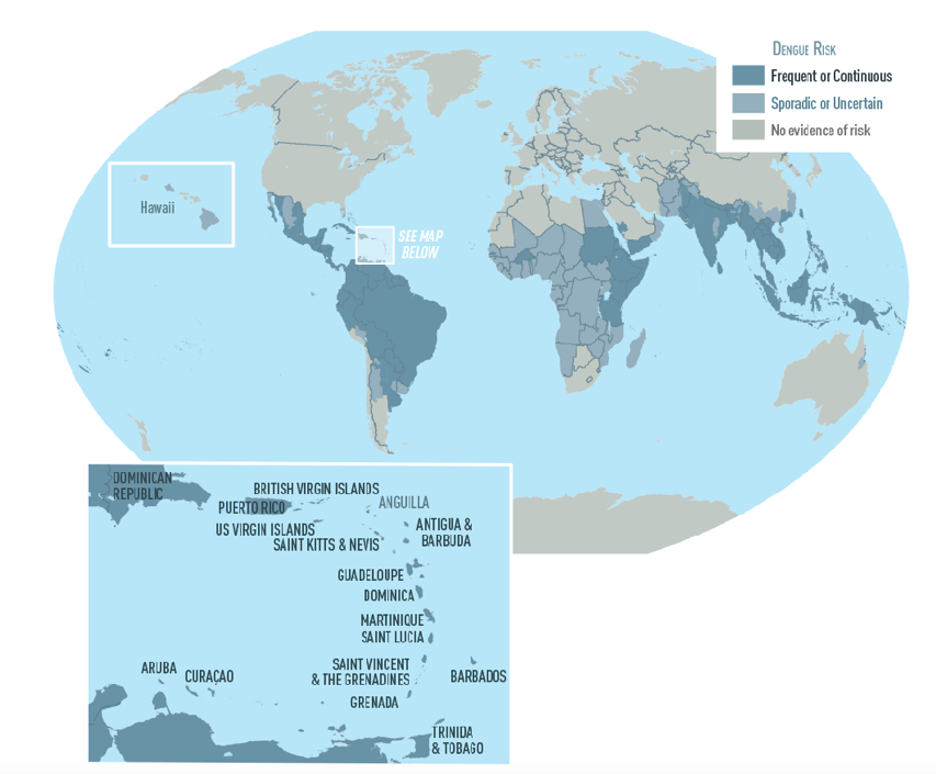
Figure 5 | Global distribution of Dengue, bbtained from https://www.cdc.gov/dengue/areaswithrisk/around-the-world.html.
Chikungunya
- Vector (mosquito)
- Aedes aegypti
- Aedes albopictus
- Agent
- ssRNA virus
- Alphaviridae family
- Reservoir
- Humans and primates
- Transmission
- Bite from infected Aedes mosquito
- Bloodborne
- Vertical (perinatal highest risk)
- Not found in breastmilk
- High risk: neonates, age > 65, diabetes, CAD
- Presentation
- 3 – 28% asymptomatic
- Sudden-onset high fever and joint pain
- Similar to Dengue
- Viral illness: headache, myalgia, arthritis, conjunctivitis, nausea, vomiting, maculopapular rash
- Fever can be biphasic
- Arthralgias
- Joint pain can be debilitating
- Multiple joints, bilateral and symmetric involving hands and feet
- Rash
- Usually occurs after the onset of fever
- Trunk and extremities > face, palms and soles
- Severe illness is rare
- Chronic immune symptoms may persist
- Diagnosis
- History: travel, outbreaks, clinical presentation
- Labs: thrombocytopenia, lymphopenia, elevated creatinine, elevated LFTs
- Serology:
- Virus-specific IgM and IgG
- Viral culture or NAAT on serum
- after 1 week of symptom onset
- Need convalescent-phase samples if acute phase negative
- Treatment
- Supportive: rest, fluid, analgesics, antipyretics
- Acetaminophen first line until Dengue ruled out
- Can use NSAIDs in Chikungunya
- As patients can often have a chronic/long course of illness, the diagnosis is helpful for therapeutic clarity
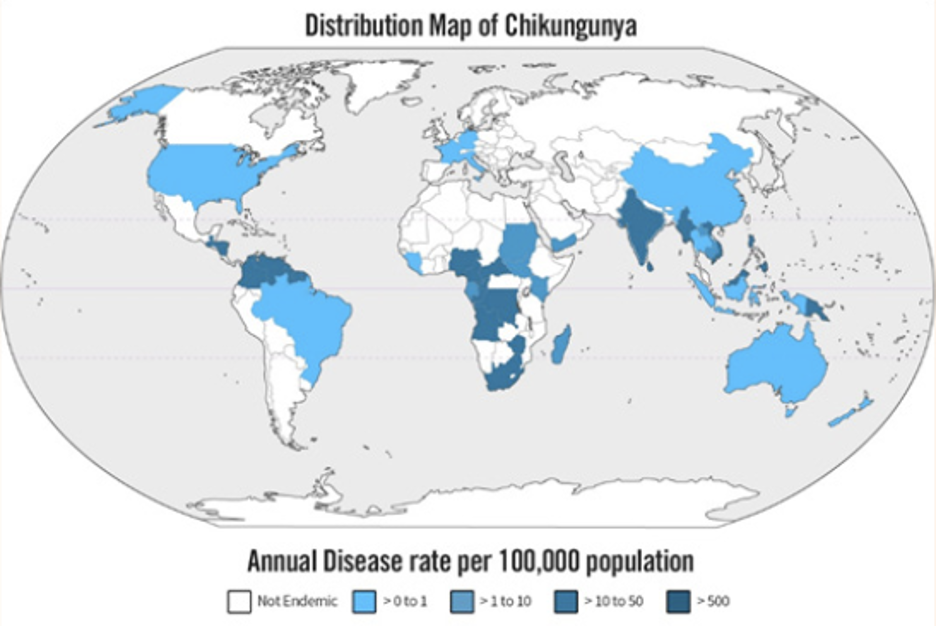
Figure 6 | Worldwide distribution of Chikungunya outbreaks from 2000 – 2015. Obtained from Diop et al (2015)6
Zika virus
For a deep dive into Zika, please refer to the Blog post by Dr. Julia Traer here. Even though media sensationalism of Zika has died down, this disease has certainly not gone away, so we need to maintain a high index of suspicion.
- Vector (Mosquito)
- Aedes aegypte
- Aedes albopictus
- Agent
- ssRNA virus
- Flavivirus
- Transmission
- Bite from mosquito
- Sexually transmitted
- Intrauterine
- Perinatal
- Human milk: risk unknown
- Laboratory
- Transfusion-associated
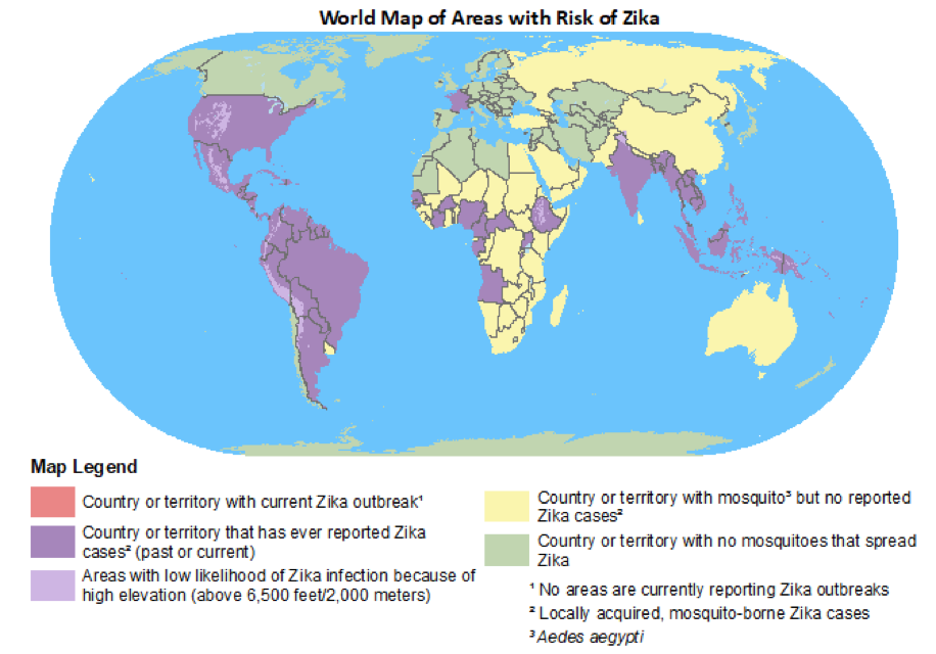
Figure 7 | Worldwide distribution of Zika. Obtained from https://wwwnc.cdc.gov/travel/files/zika-areas-of-risk.pdf.
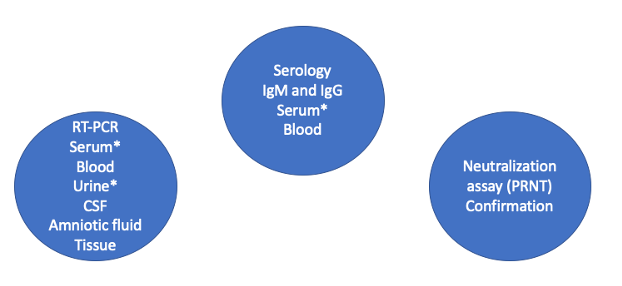
Figure 8 | Summary of diagnostic tests for Zika virus. Send blood and urine for RT-PCR. Send blood for serology. If either test is positive, a the PRNT neutralization assay will be performed for confirmation.
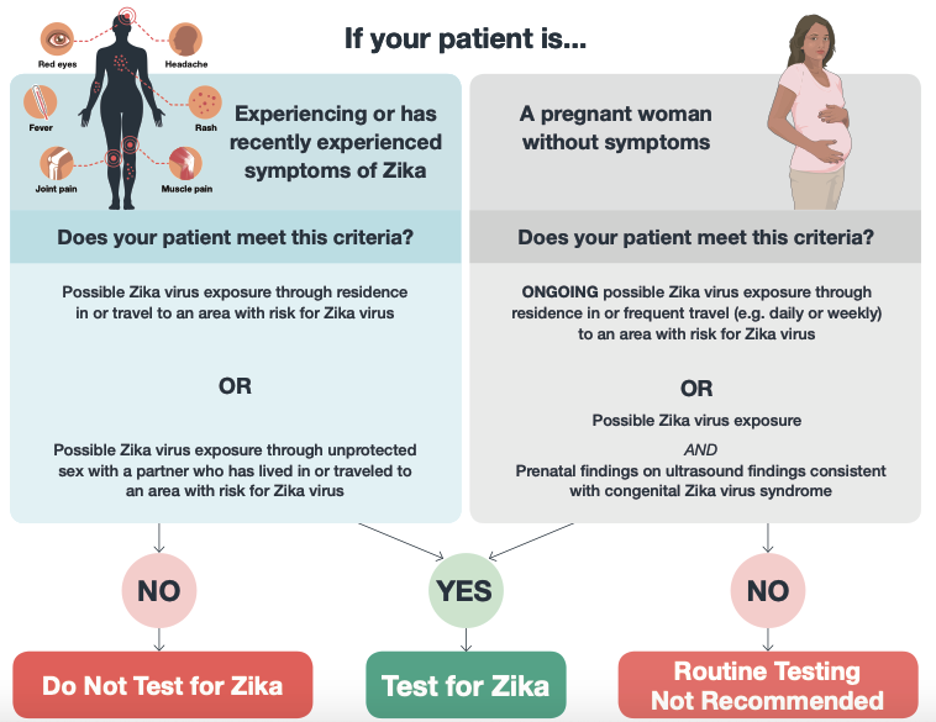
Figure 9 | Infographic obtained from https://www.cdc.gov/zika/pdfs/when-to-test-zika.pdf. Guidelines may be subject to change.
- Treatment
- Supportive care
- Avoid NSAIDs until Dengue ruled out
- No vaccine
- No countries with current outbreaks (September 17, 2020; subject to change).
- In the ED at The Ottawa Hospital for a patient suspected of having Zika:
- Draw blood work and urine
- Complete 2 requisitions (may be subject to change)
- General Requisition: https://www.publichealthontario.ca/-/media/documents/lab/general-test-requisition.pdf?la=en
- Zika-specific requisition: https://www.publichealthontario.ca/-/media/documents/lab/zika-virus-intake.pdf?la=en
- Refer to Tropical Medicine Clinic, or infectious diseases
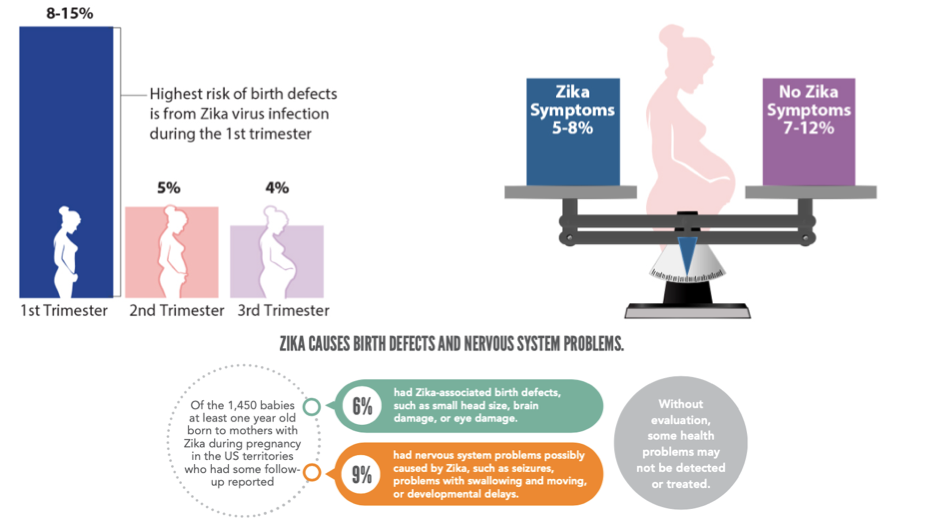
Figure 10 | Summary of literature on initial Zika outbreak. Infographics obtained from https://www.cdc.gov/pregnancy/zika/data/index.html.
A few quick words about PREVENTION…
- The best “treatment” for these diseases is prevention
- Mosquito repellant, covering clothing, bed nets
- Aedes are day biters
- Anopheles are night biters
- Ticks
- Resistant clothing
- Hats
- Skin exam
- Travel clinic before travel
- Vaccinations
- Malaria prophylaxis
- Avoiding travel if outbreaks
Resources for Clinicians
- CDC webpage: https://www.cdc.gov
Go to Travelers’ Health > Destinations > For Clinicians > Select Country.
- CDC Yellow Book, 2002. https://wwwnc.cdc.gov/travel/page/yellowbook-home
Select Table of Contents
Chapter 4 has Travel-Related Infectious Diseases
Tables in the side column has useful information. For example, Table 11-04 has typical presentations for tropical illness: https://wwwnc.cdc.gov/travel/yellowbook/2020/posttravel-evaluation/fever#5763
- Test Information Index site on Public Health Ontario. https://www.publichealthontario.ca/en/laboratory-services/test-information-index
This website has information for nurses on what samples to send for each of the vector-borne illnesses. For clinicians, it also has information on the type of test done and the turnaround time.
- Tropical Medicine Clinic in Ottawa
In EPIC, under ambulatory referral, type infectious diseases, select “Tropical Medicine”
1. Ho, Michael. What we know about Lyme Disease [online]. Available from https://emottawablog.com/2016/11/what-we-know-about-lyme-disease/. Accessed August 13 – September 10, 2020.References
2. CDC. Lyme Disease. Available from https://www.cdc.gov/lyme/index.html. Accessed August 13 – September 10, 2020. 3. Minnesota Lyme Association [online]. Available from https://mnlyme.org/about-lyme-disease/overview/ Accessed August 14, 2020.
4. Ogden, N. H., Lindsay, L. R., Morshed, M., Sockett, P. N., & Artsob, H. (2009). The emergence of Lyme disease in Canada. CMAJ, 180(12), 1221–1224.
5. Steere, A. C., Strle, F., Wormser, G. P., Hu, L. T., Branda, J. A., Hovius, J. W. R., et al. (2016). Lyme borreliosis. Nat Rev Dis Prim, 2(1), 586–19.
6. Tiny Predators in the Park: 1 out of 3 ticks tested in new Ottawa study carry Lyme Disease. (2020) [online]. Available from https://med.uottawa.ca/en/news/tiny-predators-park-1-out-3-ticks-tested-new-ottawa-study-carry-lyme-disease. Accessed August 24, 2020.
7. Walls et al. (2018) Rosen’s Emergency Medicine. (9th Edition) Philidelphia PA/USA: Elselvier
8. UpToDate. Lyme Disease [online]. Available from https://www.uptodate.com/contents/clinical-manifestations-of-lyme-disease-in-adults?search=lyme%20disease&source=search_result&selectedTitle=1~150&usage_type=default&display_rank=1. Accessed August 25, 2020.
9. Gasmi, S., Ogden, N. H., Lindsay, L. R., Burns, S., Fleming, S., Badcock, J., et al. (2017). Surveillance for Lyme disease in Canada: 2009–2015. Canada Communicable Disease Report, 43(10), 194–199.
10. Public Health Ontario. Ottawa Algorithm for Lyme Disease (2019) [online]. Available from https://www.ottawapublichealth.ca/en/professionals-and-partners/resources/Documents/Ottawa-Algorithm-for-Lyme-Disease_July2019.pdf. Accessed August 25, 2020.
11. CDC. Malaria [online]. Available from https://www.cdc.gov/parasites/malaria/index.html. Accessed August 13 – September 10, 2020.
12. CDC. Yellow Book (2020) [online]. Available from https://wwwnc.cdc.gov/travel/page/yellowbook-home. Accessed August 13 – September 10, 2020.
13. CDC. Malaria Life Cycle [online]. Available from https://www.cdc.gov/malaria/about/biology/index.html. Accessed August 20, 2020.
14. World Health Organization. World Malaria Report (2019) [online]. Available from https://www.mmv.org/newsroom/publications/world-malaria-report-2019?gclid=CjwKCAjwkoz7BRBPEiwAeKw3q9KxibQ9Snc7Iwg07NTuuQR7udMvDEoLS-6N1rWpiv_qhQtygNfl3RoCiCMQAvD_BwE. Accessed August 20, 2020.
15. Infectious Diseases and Pharmacy, The Ottawa Hospital. Malaria Binder (2019).
16. CDC. African Tick Bite Fever. [online] Available from https://wwwnc.cdc.gov/travel/diseases/african-tick-bite-fever. Accessed August 13 – September 10, 2020.
17. Cazorla C, Socolovschi C, Jensenius M et al (2008). Tick-borne Diseases: Tick-borne Spotted Fever Rickettsioses in Africa. Infectious Disease Clinics of North America 22(3): 531 – 544.
18. Faccini-Martinez A, Garcia-Alvarez L, Hidalgo M et al (2014). Syndromic classification of rickettsioses: an approach for clinical practice International Journal of Infectious Diseases. 28: 126 – 139.
19. CDC. African Sleeping Sickness. [online] Available from https://wwwnc.cdc.gov/travel/diseases/african-sleeping-sickness-african-trypansosomiasis Accessed August 13 – September 10, 2020.
20. Lundkvist, G. B., Kristensson, K., & Bentivoglio, M. (2004). Why Trypanosomes Cause Sleeping Sickness. Physiology, 19(4), 198–206.
21. CDC. African Sleeping Sickness [online]. Available from https://www.cdc.gov/parasites/sleepingsickness/diagnosis.html. Accessed August 31, 2020.
22. CDC. African Sleeping Sickness [online]. Available from https://www.cdc.gov/parasites/sleepingsickness/health_professionals/index.html#tx Accessed August 13 – September 10, 2020.
23. CDC. Dengue [online]. Available from https://www.cdc.gov/dengue/. Accessed August 13 – September 10, 2020.
24. CDC. Dengue [online]. Available from https://www.cdc.gov/dengue/areaswithrisk/around-the-world.html. Accessed September 1, 2020.
25. CDC. Chikungunya [online]. Available from https://www.cdc.gov/chikungunya/Accessed August 13 – September 10, 2020.
26. Diop D, Meseznikov G, and Sanicas M (2015). Chikungunya outbreaks from 2000 – 2015: A Review. MOJ Public Health; 2(6): 43 – 49. 27. CDC. Zika [online]. Available from https://www.cdc.gov/zika/Accessed August 13 – September 10, 2020.
28. Traer, Julia. Zika Virus – What we know and what we don’t [online]. Available from https://emottawablog.com/2017/05/zika-virus-what-we-know-and-what-we-dont/. Accessed September 2, 2020.
29. CDC. Zika [online]. Available from https://wwwnc.cdc.gov/travel/files/zika-areas-of-risk.pdf. Accessed September 2, 2020.
30. CDC. When to test Zika [online]. Available from https://www.cdc.gov/zika/pdfs/when-to-test-zika.pdf. Accessed September 2, 2020.
31. CDC. Data and Statistics on Zika in Pregnancy [online]. Available from https://www.cdc.gov/pregnancy/zika/data/index.html. Accessed September 2, 2020.




Trackbacks/Pingbacks