Spiritualism represents an important aspect within the domains of wellness. Now, spiritualism is a very personal and individual thing, but having some element of spiritualism has demonstrated benefits to one’s mental health, and our personal philosophies can help shape how we experience the world, and as a result, how medicine can impact us.
When Voyager I had past Saturn and was heading into deep space, NASA turned Voyager around to take a picture of Earth. That picture lead to a rather famous Carl Sagan monologue on our insignificance as a ‘pale blue dot in the great enveloping cosmic dark‘. While seemingly grave, this represents a strong pillar in my core philosophy.

It represents this idea that in the grand scheme of the cosmos, we are seemingly insignificant, and while this idea is scary, it represents an understanding that as a species we became self-aware to realize that this story of the Universe isn’t about us.
Optimistic Nihilism
But, if we’re taking about wellness within medicine, what does optimistic nihilism have to do with anything? How is this helpful?
We have to remember that it isn’t the medicine that hurts people, it’s the day to day grind. The system issues; trying to arrange outpatient antibiotics for a patient, wrist fractures in elderly patients with walkers, social admissions etc.
Optimistic nihilism represents a value statement around ones efforts to advocate for patients. Recognizing that we are all small cogs in a large (medical) machine means it is important to combat morale distress by anchoring in a patients best interests. Of course, its hard when the ‘system’ pushes back against your efforts – and inevitably, residents feel this strain the most because they live it more frequently.
While it may be unsettling to wrestle with the idea of our own insignificance, when you isolate any one individual on Earth, you find hopes, dreams, a childhood and lived experience. Knowing that nothing matters, for me, is protective, because it allows every place to become the center of the Universe, every moment becomes the most important and everything is the meaning of life. You get one shot at life – and that’s scary, but that knowledge also sets you free.
If our life is all we get to experience, then that’s the only thing that matters. Since there are no principles (other than physics) within our Universe; then we get to dictate its purpose, and our purpose within in.
We cannot control all the variables around us, so there is no point commiserating over the things we can’t control, and rather focus our energy into things that we can control, because medicine breeds within us a sense of nihilism, and causes us to internalize the systems problems within us. This can eventually cause a dangerous internalization of things as a ‘me’ problem, rather than a ‘system problem’.
Recognizing that on any given shift, in any given moment, all I can do is advocate for the patient in front of me, and help them to navigate the system comes from my personal philosophy as an optimistic nihilist – because that is what works for me. We all need to identify our own personal reflections of this based on the lens through which we each see the world.
We are not different people at home versus at work. Sure, we modify behaviours, but being human is central to what we give to medicine.
Medicine is tough right now, but when we’re cognizant of the variables that we can control, and what we can do to control and optimize our own occupational wellness – we can make it better for ourselves.
Mindfulness
Mindfulness may often be considered one of the fluffier concepts in medicine, and I’ll confess I was quite skeptical myself. Many think or assume that mindfulness means to control the mind or to meditate; but its more nuanced than this.
The physiologic rationale for mindfulness is that we’re constantly encountering both micro and macrostressors on a daily basis; and our reaction to microstressors contributes to a state of adrenal activation. That throughout any given day, many of us feel in our lives or on shifts that we’re fighting a bear – so its no wonder we feel unwell.
Mindfulness teaches us to avoid the adrenal stimulation we feel when we encounter microstressors, and imparts us to recognize when we’re encountering situations over which we have no control.
A great analogy by Andy Puddicombe for mindfulness is to envision that you are sitting on the side of the road, watching cars go by, and those cars are your thoughts. The point of the exercise is just to sit at the side of the road and watch those thoughts, but inevitably, many of us try to stop the cars, or run alongside and start following a few of them – forgetting that the point of the exercise is just to sit there. This, of course, takes practice. Deliberate practice.
In medicine, we practice everything; procedures, protocols, simulation. We cannot become procedurally competent at HALO procedures without deliberate practice, and if wellness is an important idea (it is) then it too, requires deliberate practice.
I started off just with brushing my teeth. 4 minutes a day; I would brush my teeth and practice being mindful; turning of my physiologic responses, and just being present in that moment,. I wouldn’t be on my phone, or ruminating about my day, or planning tomorrow. When my mind would wander, or I’d ‘start following a car’, I’d come back to the brush on my teeth and how that felt, and that would anchor me. After a while of this practice, I was able to integrate it into more and more moments in my day.
I got rid of my road rage this way; recognizing that it was a negative physiologic response to a variable that I couldn’t control. I was only hurting myself with my response, so now, instead, I just take a deep breath – and I’m settled.
I began to practice meditating – 5 to 10 minutes at a time. I’m not very good at it, but I still practice it anyways because I notice a benefit. Before every night shift, I cuddle with my dog and we both do some deep breathing (surprisingly, he joins me and mimics my breath), and its very anchoring for me. Unsurprisingly, the more I practice, the better I get at it.
I’m still working on it – but I’ve started to engage it more at work; recognizing my negative physiologic responses to microstressors at work. Difficult consultant or patient interactions, frustrations within the system; I am working within myself to mitigate negative physiologic responses to morale distress because it is very protective.
Have I noticed a difference? Absolutely, and literature would support that feeling.
Feel your Feelings
When I was in residency, I recall a traumatic case of a young person who was murdered. I had to break the news to his wife, who was holding a 17 month old at the time, and I will never forget the screams in that room. I was rattled.
After the shift, I went out to breakfast with my staff, who said something to the effect of
“why are you still on about that? People die all the time, get over it. You need to compartmentalize things or you’ll never survive in this job”.
I remember feeling appalled, and never wanted myself to feel that jaded or nihilistic. I actually think that it is important and healthy to feel your feelings. I’ve actually come to adopt the opposite philosophy, because I do not think that you can be a good ER Physician if you are going to be that blaise about the loss of human life. Certainly we need to compartmentalize aspects of our job, so that we don’t take most things home with us – but some cases can, and should stick with you.
A great tangential piece of advice that goes with this, however, is that when something bad happens, or doesn’t go your way; you get disappointing news etc. Feel your feelings (whatever that means for you) but set at timer on it; 5, 10 minutes, maybe 1-2 weeks, whatever it is, and allow yourself to have those feelings, but once that timer goes off, you have to say “Cant change it” and move on. Learn from it, reflect from it, but don’t let it ruminate.
Routine
My acknowledgement that I cannot stress about variables I cannot control is important because it places an emphasis on addressing variables that I do have control over. I place additional emphasis on these variables, because while I cannot control how many people are in the waiting room on any given day, I can control how well fed/caffeinated I am.
My post work routine has become very deliberate. When I leave work, I like to enjoy my drive home. I listen to music, and simply enjoy my driving experience. I am thinking about nothing else. Once I am home, I shower, and I actually spend the first few minutes debriefing my shift;
“Maybe I should’ve scanned that person..”
“I really shouldn’t swear in front of medical students”
“I think we really helped that person”
“That was a cool case”
Note that I tend to close my shift debrief with positive things, or things that I enjoyed on that shift because that is what I take home with me.
The next few minutes I spent doing some mindfulness, and then I transition into whatever I need to go do; ‘dad mode’, go to sleep, etc.
My preshift routine is also very deliberate. I do not look at the EMR (I know some people do), because I don’t find it to be particularly helpful because it is only likely to stress me out. I do, however, look to see who I am working with. Because, if I know I have two junior learners, my shift is going to be more challenging than if I have a single ER resident, or if I am working alone. So my preparation is absolutely different. I may eat a better meal, get to work a few minutes earlier (so I can have a dance party in my car) – because I want to set the tone.
Productive physicians accomplish most of their ‘extra work’ within the first 2 hours of their shifts, after that most people tend to plateau off to similar levels of productivity. If I show up to work in a good mood, I am going to be more productive in that first two hour segment, than if I do not feel well. So for me; that’s a dance party in my car, and controlling variables that I know will put me in the best headspace to do my job. I try to start my shift with some enthusiasm, because the idea of ‘faking it until you make it’ actually works.
Resilient People have Strong Relationships
Evidence would suggest that resilient people have strong relationships both at work and at home. Many would be familiar with Dr. Sara Gray’s philosophy on having a ‘failure buddy’ at work, and there is good evidence to support that idea.
I learned an important foundation to establishing strong relationships is good communication, and a willingness to be vulnerable – and allowing myself to embrace these has been tremendously helpful for my own personal wellness.
Here’s an example; around the Holidays this year, I worked a lot, and then we traveled to see family, and then I worked a lot more. My last shift in a string of shifts was a struggle, I was tired, and it was a difficult shift. I had anticipated that this would happen; and so in the first few hours of the shift, I tried to see as many people as possible to ensure that I had done my job of helping department, because the last few hours of that shift I had to coast.
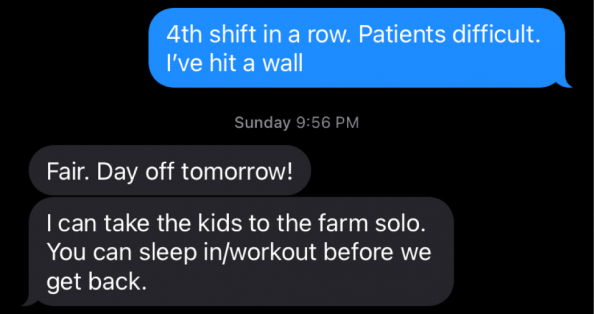
The second thing was communicating this to my wife:
Me communicating my fatigue to my wife, and her recognizing it became the difference between my battery being drained to 20%, versus sitting at 50% – I tried to combat my own wellness a priori.
This greatly aids the problem that many of us have; we often go on vacation, recharge our batteries, and one or two shifts later we’ve once again depleted it. It is important to find ways to maintain our batteries while we are existing in the day to day grind of life and work.
Conclusions
The biggest issue with occupational wellness within medicine is the lack of control. A true approach to wellness requires us to acknowledge that there are only certain variables that we do have control over, and ultimately it is our mind within our own control. Our physiologic stress response to the morale distress we encounter, to how our external world influences us is ultimately, within our control.
But controlling our responses takes work, and deliberate practice.
- Wellness isn’t fluffy BS
- It does take work
- You need perspective
- Morale distress is inevitable
- Personal agency is important and requires reflection
- Don’t stress about things that you cannot control
- Communicate
- Practice mindfulness



Trackbacks/Pingbacks